Seborrhoeic dermatitis
Your health expert: Dr Anton Alexandroff, Consultant Dermatologist
Content editor review by Pippa Coulter, Freelance Health Editor, February 2023
Next review due February 2026
Seborrhoeic dermatitis is a condition that causes a red, flaky and itchy rash on your skin. It affects areas of your skin that tend to be greasier, like your face, scalp and chest. It’s also known as seborrhoeic eczema.
About seborrhoeic dermatitis
Seborrhoeic dermatitis causes inflammation in areas of your skin that have a lot of sebaceous glands. These glands make an oily fluid called sebum, which keeps your skin supple. Areas of skin where you have lots of sebaceous glands include your face, scalp and chest. Seborrhoeic dermatitis also tends to affect areas of skin where there are skin folds. These include your armpits, under your breasts and your groin. These are areas that tend to stay moist.
Seborrhoeic dermatitis affects up to 5 in every 100 adults. Around half of adults have dandruff, which is a mild, non-inflammatory form of seborrhoeic dermatitis that affects your scalp.
It’s very common for babies to get a short-lived, mild form of seborrhoeic dermatitis. This mainly affects their scalp, where it’s known as cradle cap.
Otherwise, you can develop seborrhoeic dermatitis at any age, from puberty onwards. This is when your sebaceous glands become active. Men are more likely to get it than women.
Causes of seborrhoeic dermatitis
It’s not clear exactly why some people get seborrhoeic dermatitis. But it's thought it could be a reaction to a yeast called Malassezia, which lives on our skin. People with seborrhoeic dermatitis may have more of this yeast growing on their skin, or may be more sensitive to it.
Most people who get seborrhoeic dermatitis are otherwise healthy. But it can sometimes be associated with certain other conditions. These include:
- conditions that affect your nervous system, such as Parkinson's disease, or stroke
- a weakened immune system, for example due to human immunodeficiency virus (HIV), or taking certain medicines
- some genetic disorders, like Down’s syndrome
Your symptoms may get worse when you’re tired, stressed or generally unwell. You may also notice that your symptoms are worse when it's cold, and better in warmer weather. HIV can make symptoms more severe and harder to treat.
It’s possible that diet may play a part for some people with seborrhoeic dermatitis. But the evidence isn’t strong enough to say whether any particular foods trigger seborrhoeic dermatitis. Seborrhoeic dermatitis isn’t contagious, meaning that you can’t catch it or pass it on to another person.
Symptoms of seborrhoeic dermatitis
Symptoms in teenagers and adults
Seborrhoeic dermatitis causes red, flaky or scaly patches on your skin. The affected area may be itchy and sore. On black or brown skin, the affected areas may look darker or lighter than the surrounding skin. The most commonly affected areas include the following.
- Your scalp. Symptoms range from mild, flaky skin (dandruff) to a more severe, scalier, itchy rash which may weep.
- Your face – especially between your eyebrows, on your cheeks and in the folds at the sides of your nose. It can also affect your eyelids, making them red, swollen and flaky. This is known as blepharitis.
- Your ears. The skin inside your ear may become inflamed, as well as your outer ear and the skin behind your ear.
- Your upper chest and your back, between your shoulder blades. These areas may have round, pink or red patches with mild scaling.
- Skin folds, such as your armpits, under your breasts and your groin. Your skin here might appear pink, shiny and cracked.
As an adult, seborrhoeic dermatitis is something that you will have for life. However, your symptoms may come and go over time.
You can often deal with mild symptoms such as dandruff by yourself. You can also get advice from a pharmacist. But if your symptoms are severe or cover a lot of your skin, contact your GP for advice.
Symptoms in babies
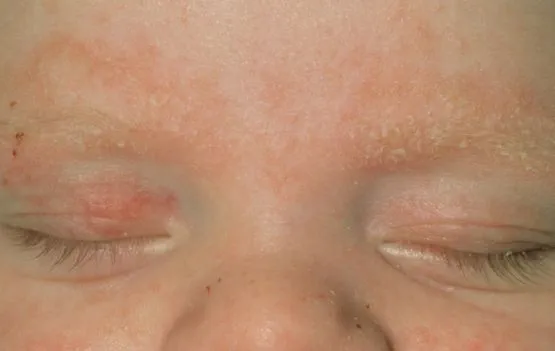
Babies often get a short-lived form of seborrhoeic dermatitis on their scalp, known as cradle cap. This causes greasy, yellow-brown, scaly patches on their scalp. Seborrhoeic dermatitis can sometimes also affect other parts of your baby’s body, including:
- their face
- behind their ears
- in skin folds
- in their nappy area
In these areas, the affected skin usually has drier, whiter scales than those on their scalp. Any itching in babies is usually mild, and is unlikely to bother your baby.
Cradle cap usually gets better by about four months of age, but it can take up to a year. If your baby just has cradle cap, you won't normally need to see a doctor for a formal diagnosis or treatment. Your health visitor may be able to give you some advice on dealing with it using over-the-counter products. But if it doesn’t improve or seems to be causing distress to your baby, contact your GP.
Diagnosis of seborrhoeic dermatitis
Your GP will usually be able to diagnose seborrhoeic dermatitis by looking at the affected areas of skin. They may also ask you some questions about your symptoms and medical history. Seborrhoeic dermatitis can look similar to a number of other skin conditions, especially psoriasis. Sometimes the two conditions can overlap.
If your GP isn’t sure whether your symptoms are due to seborrhoeic dermatitis, they may refer you to a dermatologist. A dermatologist is a doctor who specialises in identifying and treating skin conditions. They may also refer you if your symptoms are very severe or cover large areas of your body.
If you have severe symptoms of seborrhoeic dermatitis, your doctor may recommend you have an HIV test. This is because severe seborrhoeic dermatitis can be a sign of having HIV, especially if it’s come on suddenly.
Self-help for seborrhoeic dermatitis
There are things you can do to help yourself if you have seborrhoeic dermatitis. You can also usually treat cradle cap in babies yourself, without seeing a doctor.
Try to keep areas of skin affected by seborrhoeic dermatitis as clean as possible. Don’t use soap or shaving cream if these irritate your skin. Use an emollient (moisturising) soap substitute instead. You can ask your pharmacist for advice.
Your symptoms may get worse when you’re tired or stressed . Try doing things to help you relax, and avoid stress when you can. And try to avoid scratching your skin too much as this may break the skin and cause an infection.
Cradle cap
If your baby has seborrhoeic dermatitis on their scalp (cradle cap), you can treat it using the following steps.
- First use emollients (moisturisers) to soften the scales.
- Then gently brush the scales off, using a soft brush or soft-bristled toothbrush.
- Finally, wash your baby’s scalp with a baby shampoo.
Some people recommend using olive oil to soften the scales, but it’s better to use a proper emollient if you can. Ask your pharmacist if you need advice on what emollient you can use for your baby.
If your baby is affected in other areas, your GP may advise you to bathe them at least once a day using an emollient soap substitute. If it’s their nappy area that’s affected, make sure you change their nappy frequently. Use zinc and castor oil or white soft paraffin ointments as a barrier for their skin.
Seborrhoeic dermatitis treatment
There's no cure for seborrhoeic dermatitis, but treatment can help to keep your symptoms under control. You may need to keep using seborrhoeic dermatitis treatments to control your symptoms over the long term. Or sometimes, you may only need them occasionally to help with flare-ups. Be aware that your symptoms are likely to come back when you stop using the treatment.
Your GP or dermatologist may prescribe seborrhoeic dermatitis treatments. But often you can buy them over the counter at a pharmacy or from a supermarket.
Scalp seborrhoeic dermatitis
If you have scalp seborrhoeic dermatitis, your pharmacist or GP will probably recommend that you try one of the following treatments.
- Medicated anti-dandruff shampoos. These contain ingredients such as ketoconazole, selenium, coal tar or zinc pyrithione. You leave the shampoo on for 5 minutes before rinsing off. Sometimes you may need to use a descaling preparation, like coconut oil or salicylic acid, first. You can buy many of these shampoos from a pharmacy.
- Corticosteroid (steroid) gels or lotions. These are recommended if you have severe inflammation, itching and flaking. You should only use them for short periods (up to a maximum of four weeks) unless you have specific advice from your GP. This is because they can cause side-effects like thinning of your skin.
If your seborrhoeic dermatitis keeps coming back, your GP may recommend that you carry on using an antifungal shampoo once every week or once every two weeks.
If your baby has cradle cap, see our section on self-help for tips on how to treat it yourself. Your GP may prescribe an antifungal cream if your baby has cradle cap that doesn't clear up by itself.
Seborrhoeic dermatitis on your face and body
Your GP may prescribe the following treatments for seborrhoeic dermatitis on your face or body.
- An antifungal cream containing ketoconazole or another medicine. You’ll need to apply this, once or twice a day for at least four weeks to get your symptoms under control.
- An antifungal shampoo to use as a body wash.
- Medicated eardrops, if you have seborrhoeic dermatitis inside your ears.
- A steroid cream. You may be prescribed this together with an antifungal agent to reduce inflammation. You should only use steroid creams for up to two weeks, as they can cause side-effects like thinning of the skin.
- Topical calcineurin inhibitors. These include tacrolimus ointment and pimecrolimus cream. Your doctor may prescribe these instead of steroids if you need long-term treatment for inflammation.
Severe seborrhoeic dermatitis
Your GP may refer you to a dermatologist if your seborrhoeic dermatitis:
- is severe
- covers many areas of your body
- doesn’t respond to normal treatments
Your dermatologist may prescribe antifungal tablets if your rash is very severe or widespread. But this is rare.
Seborrhoeic dermatitis is a condition that makes your skin red, flaky and itchy. It’s also known as seborrhoeic eczema. It affects areas of your body where there are lots of oil-producing glands. These include your face, scalp and chest. Read the about section for more information.
Seborrheic dermatitis varies in severity from mild, flaky dandruff on your scalp to scaly, red patches on large areas of your skin. Babies can get seborrhoeic dermatitis on their scalp, known as cradle cap. This causes greasy, yellow-brown, scaly patches on their scalp. Read more in our symptoms section.
Doctors aren’t sure why people get seborrhoeic dermatitis. But it's thought to be associated with a yeast called Malassezia, which is found on our skin. People with seborrhoeic dermatitis seem to have more of this yeast, or are more sensitive to it. See the section on causes for more details.
Although studies have looked at a possible link, there’s no strong evidence that any particular foods trigger seborrhoeic dermatitis. Things that may trigger a flare-up include stress, tiredness and cold weather. See the causes section for more information.
If you have seborrhoeic dermatitis, your symptoms will usually come and go. There are certain things that can trigger a flare-up, including feeling tired, stressed or unwell. Cold weather can also trigger symptoms. You can read more on this in our causes section.
You can’t cure seborrhoeic dermatitis. In adults, it’s a disease that you’ll have for life. But symptoms can come and go over time. And there are treatments to help you get symptoms under control when you need it. See our treatment section to find out how to manage your symptoms.
Corticosteroids
Psoriasis
Psoriasis is a lifelong skin condition that causes raised patches of inflamed skin. It affects people differently and can come and go over time.
Does stress cause skin problems?
Did you know that stress and skin problems such as itching or rashes can be linked?
Did our Seborrhoeic dermatitis information help you?
We’d love to hear what you think.∧ Our short survey takes just a few minutes to complete and helps us to keep improving our health information.
∧ The health information on this page is intended for informational purposes only. We do not endorse any commercial products, or include Bupa's fees for treatments and/or services. For more information about prices visit: www.bupa.co.uk/health/payg
This information was published by Bupa's Health Content Team and is based on reputable sources of medical evidence. It has been reviewed by appropriate medical or clinical professionals and deemed accurate on the date of review. Photos are only for illustrative purposes and do not reflect every presentation of a condition.
Any information about a treatment or procedure is generic, and does not necessarily describe that treatment or procedure as delivered by Bupa or its associated providers.
The information contained on this page and in any third party websites referred to on this page is not intended nor implied to be a substitute for professional medical advice nor is it intended to be for medical diagnosis or treatment. Third party websites are not owned or controlled by Bupa and any individual may be able to access and post messages on them. Bupa is not responsible for the content or availability of these third party websites. We do not accept advertising on this page.
- Seborrhoeic dermatitis. Patient. patient.info, last edited 14 March 2022
- Seborrhoeic dermatitis. NICE Clinical Knowledge Summaries. cks.nice.org.uk, last revised July 2022
- Seborrhoeic dermatitis. British Association of Dermatologists. www.bad.org.uk, updated April 2018
- Sebaceous gland. Encyclopedia Britannica. www.britannica.com, last updated 29 December 2022
- Tucker D, Masood S. Seborrheic dermatitis. StatPearls Publishing. www.ncbi.nlm.nih.gov/books, last updated 1 August 2022
- Seborrhoeic dermatitis. BMJ Best Practice. bestpractice.bmj.com, last reviewed 4 December 2022
- Sanders MGH, Pardo LM, Ginger RS, et al. Association between diet and seborrheic dermatitis: a cross-sectional study. J Invest Dermatol 2019; 139(1):108–14. doi: 10.1016/j.jid.2018.07.027
- Personal communication, Dr Anton Alexandroff, Consultant Dermatologist, 10 February 2023
- Conditions for which over-the-counter items should not routinely be prescribed in primary care: Guidance for CCGs. NHS England. www.england.nhs.uk, 29 March 2018



