Cataracts
- Professor Simon Taylor, Consultant Ophthalmic Surgeon
A cataract is when the lens of your eye gets cloudy so you can’t see through it as well. Cataracts can make your vision blurred or misty over time. Cataracts often build up slowly over several years.
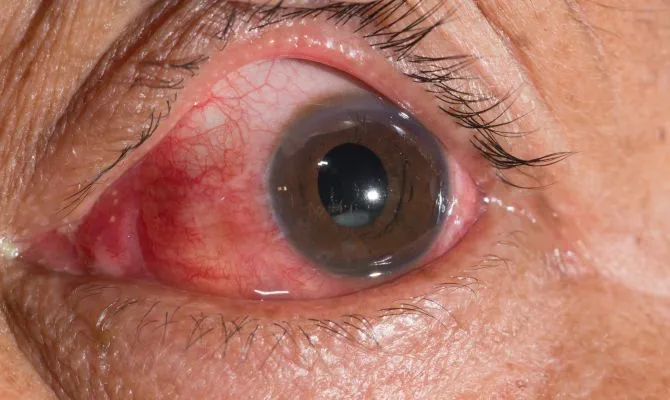
About cataracts
Your lens is near the front of your eye just behind your iris (the coloured part of your eye). It’s normally see-through and helps you to see things clearly. Your lens directs light rays onto your retina (the back of your eyeball) to form a picture, which is then sent to your brain.
If you have a cataract, proteins in the lens of your eye are changing over time, which causes your lens to become cloudy. This is called a cataract. Cataracts usually form over a long period of time and your eyesight gets worse very slowly. You're more likely to develop cataracts as you get older. You can get a cataract in just one eye or both of them.
The only way to treat a cataract is to replace your cloudy lens with an artificial one, called an intraocular lens. This will usually last for the rest of your life. Your decision on whether or not to have a cataract operation may depend on how much your cataracts affect your daily life. Some cataracts may not change your vision at first. But you may decide to have cataract surgery if your cataracts are stopping you from reading or driving safely in low light.
Types of cataracts
There are different types of cataract that can affect adults. These form in different parts of the lens in your eye.
- Nuclear cataracts. These form in the middle of your lens and are more common as people get older.
- Cortical cataracts. The cloudiness starts on the outside of your lens. It then slowly moves towards the centre. These cataracts don’t always cause symptoms unless you’ve had them for a long time.
- Posterior subcapsular cataracts. These form at the back of your lens. They’re more common in younger people.
Some babies are born with cataracts, which are called congenital cataracts.
Causes of cataracts
Cataracts are caused by changes in your eye that make your lens cloudy. The main cause of cataracts is age – changes which usually happen naturally as you get older. But some other things may make you more likely to get cataracts. These include:
- diabetes
- an injury to your eye
- bad inflammation (swelling and redness) of your eye (uveitis)
- exposure to ultraviolet (UV) light in sunlight over a long time
- taking medicines called corticosteroids in high doses or for a long time
- smoking
- drinking too much alcohol
- a family history of cataracts
Symptoms of cataracts
If you have a cataract, you may not notice any symptoms at first. Cataracts aren’t usually painful. Your symptoms will depend on:
- the size of your cataract
- where it is in your lens (the type of cataract you have)
- whether you have a cataract in one or both of your eyes
Cataracts symptoms include:
- cloudy or blurred vision – for example, finding it harder to read, watch television or recognise faces
- trouble coping with bright light, including light from the sun
- problems with glare, especially when you’re driving at night
- difficulty seeing colours – shades of blue, in particular, may seem washed out or faded
- seeing ‘halos’ around lights
If you have cataracts, you may notice that the prescription for your glasses or contact lenses changes more often than usual.
Some of these symptoms could be caused by problems other than cataracts – for example, diabetes or glaucoma. So if you notice any changes to your eyesight, make an appointment with your local opticians. An optometrist can check the health of your eyes, test your sight and prescribe glasses and contact lenses if you need them.
Diagnosis of cataracts
If you think you have symptoms of cataracts, get your eyes tested by an optometrist. They’ll look into your eyes using a special instrument called an ophthalmoscope.
If you have a cataract, your optometrist will be able to see that the lens of your eye is cloudy. Your lens may look a different colour when they shine a bright light into your eye – it may be a yellow–brown colour or look grey or white.
Your optometrist may then refer you to an ophthalmologist (a doctor who specialises in eye health) for treatment. But you don’t always need treatment if the cataract doesn’t interfere with your sight.
Your optician may notice you have a cataract during a routine eye test. This is because the changes in your lens can happen slowly over many years – so you may not have noticed any symptoms.
Self-help for cataracts
If your cataracts aren’t very bad, you may be able to try some things to help you see more clearly.
- Stronger glasses or contact lenses may help. Your optometrist will change your prescription if your vision is getting worse.
- To make it easier to read, don’t sit too close to a light source such as a lamp.
Because cataracts are likely to get worse over time, these measures will only work for a short while. You’ll need to have regular eye examinations to check your cataracts and make sure your vision isn’t getting worse. If your eyesight keeps getting worse, your optometrist may recommend that you have cataract surgery.
Cataract treatment
Removing your cataract in a cataract operation is the only way to get your vision back to normal. Your ophthalmologist will talk to you about whether or not cataract surgery is right for you. This will depend on lots of things including how much your cataract is affecting your daily activities.
Cataracts affect everyone differently. If you don’t read much, you may not be bothered if your cataracts make it harder for you to read. You may decide to wait longer for a cataract operation. But if you drive a lot, especially at night or you need to see details clearly, you may decide to have a cataract operation sooner.
Most cataracts are removed in an operation called phacoemulsification under local anaesthesia.
Your surgeon will usually only operate on one eye at a time. If you have cataracts in both eyes, they may treat your eye with the worst vision first. You’ll have the second cataract operation once your surgeon knows that the first one worked well.
But your surgeon may recommend having a cataract operation on both eyes at the same time. This could be because you’re unlikely to have any serious eye complications after cataract surgery so it’s safe for you to have just one operation. Or it may be safer for you to have one cataract operation rather than two. Perhaps because you need to have a general anaesthetic rather than a local one, and there’s a risk you may react badly to it. Speak to your surgeon to find out if this is an option for you.
Your surgeon can use different types of artificial lens in the operation. They come in different strengths, just like the lenses in glasses. They also vary in how well they focus on objects at different distances.
After surgery
Most people don’t have any sight problems after a cataract operation. But you may need to wear reading glasses afterwards, although new lenses are being developed to correct this.
If your vision doesn’t get better after surgery, this may be because you have another eye condition, such as glaucoma or age-related macular degeneration. Sometimes, your ophthalmologist can’t diagnose these other eye conditions until your cataract has been taken away.
Sometimes, a cataract operation can cause a condition called posterior capsule opacification. This may make your vision cloudy, but it’s not the same as a cataract. It’s caused by a thickening of your natural lens casing – the part of your eye that holds your lens in place. This lens casing isn’t usually taken away during surgery.
If you have this condition, your doctor will offer you a minor laser procedure to fix your vision. This can usually be done in an outpatient clinic and only takes a few minutes.
Complications of cataracts
Cataracts may stop you doing some activities you enjoy, such as reading, driving or watching TV. If your cataract isn't treated, you may eventually not be able to see properly at all.
If your cataracts are affecting your vision, you may be more likely to have an accident or a fall. But cataracts are normally diagnosed and treated well before they affect your vision badly.
Cataracts can make it harder for your ophthalmologist to diagnose other long–term eye conditions, such as glaucoma. If you have diabetes, you’ll need to have eye tests regularly to check your eyes are healthy.
But if you have a cataract as well as diabetes, these eye tests may not work so well. This is why you may be advised to have the cataract taken away.
Sometimes cataracts can cause a condition called angle–closure glaucoma. This may happen if a cataract makes your lens swell (get bigger).
If you have angle–closure glaucoma, the pressure in your eye increases very quickly. This can cause sudden, strong pain in your eye, blurred vision and a red eye. You may also have a headache and feel sick.
If you have any of these symptoms, get medical help straight away to make sure your sight isn’t permanently damaged.
Prevention of cataracts
You can’t prevent cataracts. But you may be able to reduce your chances of getting one by:
- staying safe in the sun and wearing UV-blocking sunglasses to protect your eyes from sunlight
- stopping smoking
- drinking less or no alcohol
- if you have diabetes, making sure your blood sugar levels are well controlled
To stop your cataracts getting very bad:
- have regular check–ups with your optometrist or ophthalmologist
- consider having cataracts surgery if they recommend it
There isn't anything you can do to stop your cataracts from getting worse. But it’s a good idea to protect your eyes from the sun by wearing UV-blocking sunglasses. Make sure you have regular check-ups with your optometrist or ophthalmologist so they can monitor your condition. And consider having cataract surgery if they recommend it.
For more information, see our section on self-help for cataracts.
Cataracts can be serious if they get worse and you don’t get treatment. Cataracts can potentially cause blindness but they’re normally diagnosed and treated well before they affect your vision badly. It’s important to have regular check-ups with your optometrist or ophthalmologist to monitor your cataracts so you can get treatment when you need it.
Some people can still drive with cataracts. This will depend on how bad your cataract is and if your sight is still within the legal limits for driving. If your cataracts affect your driving, you will need to contact the Driver and Vehicle Licensing Agency (DVLA). Check with your optometrist before you drive.
Cataracts affect people in different ways so it’s hard to predict how quickly they’ll affect your vision. Your eyesight will usually get worse very slowly, sometimes over a number of years. If you have an underlying medical condition such as diabetes, your vision may be affected more quickly.
Your specialist doctor (ophthalmologist) will usually recommend to have your cataracts taken out when they start to affect your daily life. Cataracts can stop you seeing properly and may make you more likely to fall or have an accident. The only way to get your vision back to normal is to have an operation. Your ophthalmologist will talk to you about whether or not cataract surgery is right for you. This will depend on lots of things including how much your cataract is affecting your daily activities. For more information, see our section on cataract treatment
At first, you may not notice any cataract symptoms. Or you may struggle to see properly when you try to read, watch television or even recognise faces. You may find it harder to drive at night because there’s too much glare. For more information, see our section: symptoms of cataracts
Cataract surgery
Corticosteroids
Local anaesthesia
Local anaesthesia involves numbing a small part of your body with a medicine called a local anaesthetic to stop pain during and after surgery.
Did our Cataracts information help you?
We’d love to hear what you think.∧ Our short survey takes just a few minutes to complete and helps us to keep improving our health information.
∧ The health information on this page is intended for informational purposes only. We do not endorse any commercial products, or include Bupa's fees for treatments and/or services. For more information about prices visit: www.bupa.co.uk/health/payg
This information was published by Bupa's Health Content Team and is based on reputable sources of medical evidence. It has been reviewed by appropriate medical or clinical professionals and deemed accurate on the date of review. Photos are only for illustrative purposes and do not reflect every presentation of a condition.
Any information about a treatment or procedure is generic, and does not necessarily describe that treatment or procedure as delivered by Bupa or its associated providers.
The information contained on this page and in any third party websites referred to on this page is not intended nor implied to be a substitute for professional medical advice nor is it intended to be for medical diagnosis or treatment. Third party websites are not owned or controlled by Bupa and any individual may be able to access and post messages on them. Bupa is not responsible for the content or availability of these third party websites. We do not accept advertising on this page.
- Cataracts. BMJ Best Practice. bestpractice.bmj.com, last reviewed 6 January 2024
- Understanding cataracts. Royal National Institute of Blind People (RNIB). rnib.org.uk, produced July 2022
- Cataracts and cataract surgery. Patient. patient.info, last updated 14 December 2021
- Cataracts. Royal National Institute of Blind People (RNIB). www.rnib.org.uk, last reviewed 10 February 2023
- Nizami AA, Gulani AC. Cataract. StatPearls Publishing. www.ncbi.nlm.nih.gov , last updated 5 July 2022
- Ophthalmology. Oxford Handbook of General Practice. Oxford Academic. academic.oup.com, published online June 2020
- Cataract. MSD Manuals. msdmanuals.com, reviewed/revised January 2024
- Cataracts. NICE Clinical Knowledge Summaries. cks.nice.org.uk, last revised August 2022
- Cataracts in adults: Management. National Institute for Health and Care Excellence (NICE). www.nice.org.uk, published 26 October 2017
- Eyes. Oxford Handbook of Geriatric Medicine. Oxford Academic. academic.oup.com, published online February 2018
- Zamora-de La Cruz D, Bartlett J, Gutierrez M, et al. Trifocal intraocular lenses versus bifocal intraocular lenses after cataract extraction among participants with presbyopia. Cochrane Database of Systematic Reviews 2023, Issue 1. doi: 10.1002/14651858.CD012648.pub3
- Posterior capsule opacification. Royal National Institute of Blind People (RNIB). www.rnib.org.uk, last reviewed 1 September 2022
- Diabetes – type 2. NICE Clinical Knowledge Summaries. cks.nice.org.uk, last revised November 2023
- Diabetic eye screening: Slit lamp examination explained. NHS England. www.gov.uk, updated 27 July 2022
- Glaucoma and ocular hypertension. Patient. patient.info, last updated 7 February 2022
- Angle-closure glaucoma. Patient. patient.info, last updated 11 October 2021
- Senile cataract (age-related cataract). Medscape. emedicine.medscape.com, updated 2 March 2021
- Rachael Mayfield-Blake, Freelance Health Editor



