Fungal skin infections
Your health expert: Angana Nankani, Bupa GP
Content editor review by Pippa Coulter, Freelance Health Editor, October 2023
Next review due October 2026
Fungal skin infections are common. They include athlete’s foot, ringworm, and fungal nail infections. Fungal skin infections are usually mild and easily treated. But sometimes they can be more severe or difficult to treat.
About fungal skin infections
Many different fungi and yeasts can cause infections of your skin, hair, and nails. Many fungal infections are contagious (can be spread from person to person). You can get a fungal infection in the following ways.
- Through direct contact with an infected person or animal, including pets like dogs and cats.
- Sharing items such as clothes, towels, hairbrushes or bedding with an infected person.
- More rarely, from contact with soil.
- If fungi that normally live harmlessly in or on your body grow out of control.
Fungal infections are more likely in areas of your body that are warm or moist. This means you’re more likely to get an infection if you:
- live or work in a hot or humid environment
- wear tight-fitting clothing or shoes that don’t let your feet ‘breathe’
- tend to sweat lots
- are obese with skin folds that rub against each other
You’re also more likely to develop a fungal skin infection if you:
- have a weakened immune system due to illness like HIV, or to taking medicines like corticosteroids
- have diabetes
- have other conditions affecting your skin – for example, psoriasis or eczema
Having a weakened immune system may also mean the infection is more severe and harder to treat.
Symptoms of fungal skin infections
The symptoms of a fungal skin infection depend on the type of fungus that’s caused it, and where it is. You may notice changes in your skin, hair, or nails. The fungus can affect just one area or several areas of your body. Fungal infections can also spread from one area of your body to another.
Fungal skin infections
Fungal infections of your skin can change how it looks. You may get patches of skin that are:
- red, discoloured or darker in colour
- scaly and itchy or have a fine scale, like dry skin
- sore, with pus-filled spots
Fungal nail infections
Fungal nail infections make your nail look abnormal and discoloured. Over time, they may cause pain and discomfort, which can interfere with standing, walking, or exercising.
Fungal scalp infections
Fungal infections of your scalp can cause your hair to become brittle and break off, leaving bald patches. It usually grows back after treatment.
You can find out more about different types of fungal infection and what they look like in our section on types of fungal skin infection.
Types of fungal skin infections
Here we describe some of the main types of fungal infection that can affect your skin and nails.
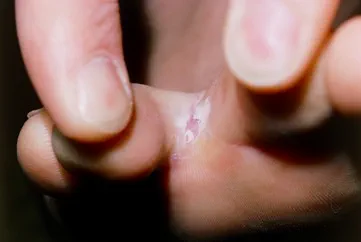
Athlete’s foot
This is the most common type of fungal infection. It affects around 7 in 10 people at some point in their lives. It’s caused by a fungus that grows in the skin between your toes and on the soles of your feet. It grows easily here because the area gets moist when your feet sweat.
Athlete’s foot can cause itchy, white, flaky patches on the skin between your toes. It may sometimes look red on white skin and cause darker patches on black or brown skin. It can cause painful cracks or fissures between your toes too. The sole of your foot can also become itchy, thickened, and scaly. You might also get blisters.
Athlete’s foot is more likely if you wear shoes that make your feet sweaty and you’re in a warm, humid environment. You can catch it by walking barefoot in shared shower or swimming areas. If you scratch the affected area, it can spread the infection to other parts of your body.
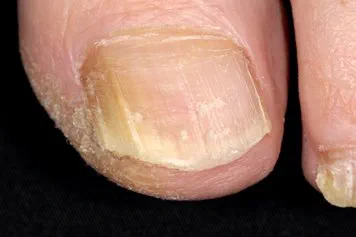
Nail infections
Fungal nail infections can affect any part of your nails. Toenails are much more likely to be affected than fingernails. The infection causes nails to discolour and become rough and crumbly. Your nail may also get thicker.
You usually get a fungal nail infection if you already have a fungal infection in another part of your body – for example, athlete’s foot. They’re also more common if you’re older or have another medical condition such as psoriasis or diabetes.
Ringworm
Despite its name, ringworm is an infection with a fungus not a worm. It gets its name because it often causes a ring-shaped rash. Ringworm infections are common, especially in children and young adults. They can affect different parts of your body.
Ringworm on your body
This causes scaly, ring-shaped patches of skin on areas of your body including your arms, legs and trunk. These may get bigger, and you may have several overlapping patches. The affected areas may look red on white skin and appear as darker patches on black or brown skin.
You can catch ringworm by touching somebody who already has it or from contact with contaminated items such as clothing or bedding. You can also catch the infection from infected animals, including cats and dogs.

Ringworm in your groin
Ringworm in your groin causes an itchy rash in your groin and around the top of your legs. This may appear red on white skin or as darker areas on black or brown skin. Also called ‘jock itch’, it’s more common in men than women.
You usually get ringworm in your groin if you have fungal infections affecting other parts of your body – for example, your feet or nails. This then spreads to your groin.
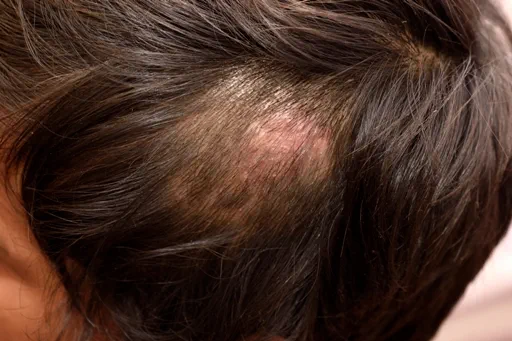
Ringworm on your scalp
You can get this at any age, but it mostly affects children. It causes scaly, itchy patches on your scalp and circular patches of hair loss. You may also notice black dots on your scalp. These are broken hair stubs. In some people, the patches become inflamed, with pus-filled spots. You may develop a crusty, pus-filled area on your scalp called a ‘kerion’.
You can get ringworm on your scalp by direct contact with someone who has the infection. You can also get it by sharing contaminated items such as hairbrushes or clothing.
Candida (yeast) skin infection
Candida is a yeast, which is a kind of fungus. It usually lives harmlessly inside your digestive system or vagina. But if conditions are right, Candida can multiply and start to cause symptoms. These yeast infections most often appear around your genitals (vagina or penis), in your mouth, or where you have folds of skin. A common name for Candida infections is ‘thrush’. In the vagina, it’s called vaginal thrush.
Candida skin infections most often affects the areas around your groin, underneath your breasts, and in your armpits. It makes the affected area sore and itchy. Your skin may become scaly and covered with a white–yellow substance. In skin folds, the skin is usually red and moist, and small pus-filled spots may appear.
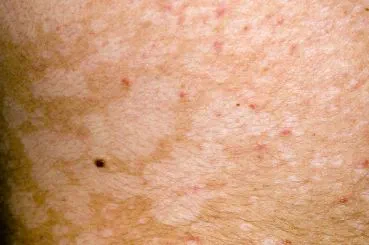
Pityriasis versicolor
This is caused by a type of yeast called Malassezia, which usually lives harmlessly on your skin. It typically affects teenagers and young adults. Pityriasis versicolor causes patches of discoloured skin with a fine scale, that are sometimes itchy. It most commonly appears on your back, chest, or upper arms but it can affect other areas. Patches can be pink, brown, red, or almost white. If you have a light skin tone, you may notice the affected area doesn’t tan as much as the rest of your skin in summer. If you have darker skin, the affected area may look paler.
Seeking help for fungal skin infections
You won’t usually need to see a GP if you have a fungal skin infection. You can usually treat it at home with over-the-counter medicines from a pharmacy. Your pharmacist will be able to give you advice. But you should see a GP if:
- the infection is affecting a large area of skin
- the infection is difficult to control or severe or over-the-counter treatments aren’t helping
- you have a scalp infection
- you’re not certain what’s causing your symptoms
- you have a weakened immune system
Your GP will usually be able to diagnose a fungal infection by examining the affected area of skin, your nail, or your scalp. They will ask you about any other symptoms you’re getting, and any risk factors you may have. Sometimes they may need to take a scrape of skin or nail for testing to confirm the diagnosis.
What should I do if I'm embarrassed to talk to my doctor?
Seeing a doctor when you're embarrassed | Watch in 2:08 minutes
Dr Naveen Puri talks about how to make it easier to see a doctor about a health issue when you are feeling embarrassed.
Hello, I am Dr Naveen Puri, I am one of the GPs within Bupa Health Clinics.
Today I want to speak to you about embarrassing problems you might have and what we can do if you attend one of our clinics.
I want you to know that many people feel embarrassed or concerned about speaking about certain things with their doctors, but I'm here to reassure you these are the kinds of things we deal with every day.
For me, looking at someone's bottom or their breasts or their genitalia is no different to looking at their nose or elbow.
And that's true for all doctors as we train for many years in these parts of the body and are very used to having these conversations with people just like you.
So what I would encourage you to do if you have any concerns from your perspective, be it a change in your bowel habit, be it a lump, a rash, a swelling. Something on your genitalia or a part of your body you're not particularly familiar with or feel uncomfortable discussing.
Please be assured your doctor has done it all before.
Some of the ways we find patients find it easier to speak to a doctor is to either tell the doctor you feel embarrassed up front. That way a doctor can make extra effort to make sure you feel comfortable.
Or some patients come to us with pieces of paper and will write the problem down and hand it to us. That way we can help with whatever is going on for you as well.
You may also find it helpful to ask for a specific doctor, someone you're familiar with in your practice. Or you might want to ask for a doctor of a specific gender, or background to your liking as well.
I'd also say, doctors do this every day so don't be alarmed if we ask you certain questions around your symptoms. It is purely so we can help you get the best outcome for your enquiry.
And then finally, feel free to use language that suits you as well. We don't expect you to know the medical words for things, or a name for your diagnosis. That's our job to find out for you.
So, take your time, see a doctor, and hopefully we can help put your mind at ease.
Self-help for fungal skin infections
Fungal infections can spread to surrounding skin and other parts of your body. There are several things you can do to help stop this and ease your symptoms.
- Wash the affected areas daily.
- Dry your skin thoroughly after washing or bathing, especially in the folds of your skin and between your toes.
- Wear loose-fitting clothes made of cotton or a breathable material.
- If you have a toenail infection, keep your feet dry and your nails short.
- Wear breathable, well-fitting shoes and cotton socks (which you should change every day). You might want to replace old footwear that could be contaminated with fungus.
- Wash your clothes, bedding, and towels often.
- Try not to scratch affected skin, as you may spread the infection to other areas of your body.
If you have ringworm, athlete's foot, or a toenail infection, you should also take measures to avoid spreading the infection to other people. These include the following.
- Don’t share personal items such as towels, clothing, brushes, or combs.
- If you have athlete’s foot or a toenail infection, don’t go barefoot in communal areas like changing rooms or swimming pools.
Candida skin infections and Pityriasis versicolor don’t spread from person to person.
If you have a fungal infection, you can still go to work. If your child has a fungal infection, they can still go to school. But you should start treatment as soon as possible and follow the measures suggested in this section to help stop it spreading to others.
For more information, see our section on preventing fungal skin infections.
Fungal skin infections treatment
You’ll usually need treatment with antifungal medicines to get rid of a fungal skin infection. If you have an infected toenail, you don’t necessarily need treatment if it’s not bothering you.
Most fungal skin infections can be treated with topical antifungals (treatments you apply directly to your skin). Sometimes you may need antifungal tablets.
Topical antifungals
Topical antifungals for fungal skin infections come in various forms. These include creams, lotions, and shampoos. Most of these are available over the counter from a pharmacist, so you don’t need a prescription from your doctor. Examples include terbinafine (Lamisil), clotrimazole (Canesten), and miconazole (Daktacort and Daktarin).
You’ll usually need to continue treatment for one to two weeks after your symptoms have gone, to make sure the infection doesn’t come back. You may need to continue topical treatment for fungal nail infection for up to a year.
Your pharmacist will be able to advise the best treatment for you. Always read the leaflet that comes with your medicine to see how to apply it and for how long. If you have any questions, ask your pharmacist for advice.
Antifungal tablets
Your GP may prescribe antifungal tablets if your fungal infection covers a large area of skin or affects your nails or scalp. Your GP may also prescribe tablets if you’ve used a topical treatment and it hasn’t cleared the infection. Antifungal tablets include terbinafine (Lamisil), itraconazole, and griseofulvin.
You may need to take the tablets for several weeks to completely get rid of the infection. This can be up to 6 months if you have a fungal nail infection. It’s important to follow the instructions that come with your medicine or the instructions your GP gives you.
Fungal infections often come back after they have been treated, especially if you are prone to getting these types of infection.
Occasionally, your GP may refer you to a specialist doctor called a dermatologist for further assessment and treatment. They may do this if you have a very severe infection, if treatment hasn’t helped, or if the infection keeps coming back. They may also refer you to a specialist if you have a weakened immune system. This can make it harder to get rid of an infection.
Prevention of fungal skin infections
You can reduce your risk of getting a fungal skin infection by taking some simple precautions.
- Dry your skin well after washing – especially in skin folds.
- Don’t walk barefoot in communal areas such as showers, saunas, and swimming pools.
- Wear loose-fitting clothes made of cotton or a breathable material.
- Don’t use other people’s towels, hats, hairbrushes, or combs.
- If you’re prone to getting athlete’s foot, alternate your shoes every two or three days to give them time to dry out. Wear open-toed shoes in hot weather.
- If you have diabetes, keep your blood sugar under control.
- If someone in your family has scalp ringworm, disinfect or replace bedding, hats, combs, and other items that may have been contaminated.
- If you suspect that your pet has ringworm, take them to the vet for treatment.
Yes. Many fungal infections can spread from person to person. This can be through direct contact or from sharing contaminated items such as clothes, bedding, or hairbrushes. If you have a fungal infection, it’s important to take measures to help stop it from spreading. You can find out more in our section on self-help.
Most fungal skin infections can be treated with antifungal creams, lotions or shampoos that you apply directly to your skin. Some fungal infections need to be treated with antifungal tablets. Speak to your pharmacist for advice on the best treatment for you. For more information, see our section on treatment.
Fungal infections can be spread between people and through contact with animals, the soil, contaminated items or floors. Some fungal skin infections – for example, thrush – are caused when your body’s own yeast (a type of fungus) grows more than usual. You may be more likely to get a fungal infection if you wear tight clothing, are overweight or have certain medical conditions. For more information, see our about section.
Fungal skin infections won’t usually go away without treatment. If they aren’t treated, they could get worse and spread to other parts of your body. You’re also more likely to pass them to other people. A fungal nail infection doesn’t necessarily need treatment if it’s not causing you any problems. Read our section on treatment to find out more.
Improving your foot hygiene alone probably won’t cure your athlete’s foot. You usually need to use topical antifungals to get rid of it. But good foot hygiene can help prevent the spread of the infection to other parts of your body. It can also help to prevent athlete’s foot from coming back and help to stop the infection from spreading to others. For more information, see our sections on self-help and prevention.
There are several different types of fungal skin infection. Some of the main ones include athlete’s foot, ringworm of your body, scalp, or groin (jock itch), nail infection, and yeast infections. Having one fungal skin infection can increase your risk of getting another because they can spread to different areas.
Antibiotics
Common vaginal infections
Psoriasis
Psoriasis is a lifelong skin condition that causes raised patches of inflamed skin. It affects people differently and can come and go over time.
Seborrhoeic dermatitis
Seborrhoeic dermatitis (or seborrhoeic eczema) is a condition that makes your skin red, flaky and itchy.
Other helpful websites
Discover other helpful health information websites.
Tools and calculators
BMI calculator
BMI, or body mass index, is one way of measuring whether you’re a healthy weight for your height.
Simply enter your details into our calculator and the result will give you an indication of whether you're a healthy weight.
Calories calculator
If you want to lose weight, you need to increase your physical activity and watch your calorie intake. Bupa's calorie calculator will help you to work out how many calories you're burning in a day.
Did our Fungal skin infections information help you?
We’d love to hear what you think.∧ Our short survey takes just a few minutes to complete and helps us to keep improving our health information.
∧ The health information on this page is intended for informational purposes only. We do not endorse any commercial products, or include Bupa's fees for treatments and/or services. For more information about prices visit: www.bupa.co.uk/health/payg
This information was published by Bupa's Health Content Team and is based on reputable sources of medical evidence. It has been reviewed by appropriate medical or clinical professionals and deemed accurate on the date of review. Photos are only for illustrative purposes and do not reflect every presentation of a condition.
Any information about a treatment or procedure is generic, and does not necessarily describe that treatment or procedure as delivered by Bupa or its associated providers.
The information contained on this page and in any third party websites referred to on this page is not intended nor implied to be a substitute for professional medical advice nor is it intended to be for medical diagnosis or treatment. Third party websites are not owned or controlled by Bupa and any individual may be able to access and post messages on them. Bupa is not responsible for the content or availability of these third party websites. We do not accept advertising on this page.
- Dermatophyte infections. BMJ Best Practice. bestpractice.bmj.com, last reviewed 8 July 2023
- Fungal nail infection. NICE Clinical Knowledge Summaries. cks.nice.org.uk, last revised April 2023
- Fungal skin infection – body and groin. NICE Clinical Knowledge Summaries. cks.nice.org.uk, last revised July 2022
- Fungal skin infection – foot. NICE Clinical Knowledge Summaries. cks.nice.org.uk, last revised June 2023
- Candida – skin. NICE Clinical Knowledge Summaries. cks.nice.org.uk, last revised July 2022
- Fungal skin infection – scalp. NICE Clinical Knowledge Summaries. cks.nice.org.uk, last revised June 2023
- Tinea pedis (Athlete's foot). MSD Manuals. msdmanuals.com, reviewed/revised September 2021
- Tinea corporis (body ringworm). MSD Manuals. msdmanuals.com, reviewed/revised September 2021
- Tinea cruris (Jock itch). MSD Manuals. msdmanuals.com, reviewed/revised September 2021
- Pityriasis versicolor. NICE Clinical Knowledge Summaries. cks.nice.org.uk, last revised July 2022
- Skin infections. NICE British National Formulary. bnf.nice.org.uk, last updated 28 June 2023
- Conditions for which over the counter items should not routinely be prescribed in primary care: Guidance for CCGs. NHS England. www.england.nhs.uk, published 29 March 2018
- Electronic Medicines Compendium. eMC. www.medicines.org.uk, accessed 10 August 2023



