Scoliosis
- Mr Ramesh Nadarajah, Trauma and Orthopaedic Surgeon
Scoliosis is when your spine permanently curves to the side. It’s often called curvature of the spine, and is most common in adolescents. You may need scoliosis treatment to prevent the curve growing bigger but it may stop naturally, especially in young children.
Diagnosing idiopathic scoliosis
The back bend test for idiopathic scoliosis | Watch in 2 minutes
This video shows how a back bend test is done. This test can be used to help diagnose idiopathic scoliosis.
About scoliosis
Scoliosis means that your spine curves in an abnormal way (more than 10 degrees). For most people with scoliosis, their spine curves in the lower back or chest, making a C or S shape. Your spine may also twist, which can pull on your rib cage and cause a hump.
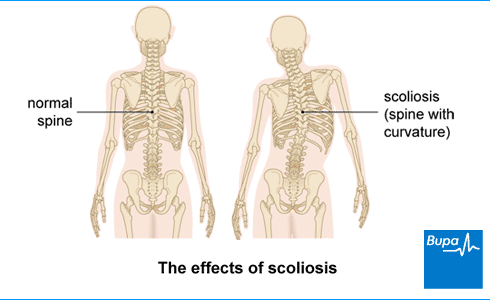
Causes and types of scoliosis
There are different types of scoliosis, depending on the age you first get it and the cause (if known).
Idiopathic scoliosis
Around nine in 10 people who have scoliosis have idiopathic scoliosis. ‘Idiopathic’ means doctors don’t know what causes the scoliois. But research shows that it often runs in families, so it may well be genetic. Idiopathic scoliosis most commonly develops between the ages of 10 and 18.
Mild scoliosis affects boys and girls equally but moderate-to-severe scoliosis is much more common in girls. The speed of growth during teenage growth spurts can affect how the spine curves, grows and develops. Once you stop growing, the curve doesn’t usually get any worse.
Early-onset scoliosis (infantile scoliosis and juvenile scoliosis)
Early-onset scoliosis affects young children. It's known as infantile scoliosis in babies and children under three, and as juvenile scoliosis if it develops between 3 and 10. It may be any of the types above. In infantile scoliosis, the spine usually curves to the left, from the chest area.
Adolescent scoliosis
Adolescent idiopathic scoliosis affects adolescents between the age of 11 and 18. Adolescent idiopathic scoliosis is the most common type of idiopathic scoliosis.
Adult scoliosis
If you had idiopathic scoliosis as a child, you may get it again because of wear and tear as you age. But normal wear of discs and joints may mean you get scoliosis for the first time as an older adult.
This is also called adult degenerative scoliosis. If you’re developing a curvature of the spine as an adult, you may find it harder to stand up straight. You may also notice that your ribcage, hip or waist sticks out. Adult scoliosis can be painful and cause shooting pain because of compressed nerves.
Congenital scoliosis
Congenital scoliosis is when you’re born with abnormalities in the structure of your spine. This means your spine doesn’t form properly and is more likely to bend as you grow. Because of the way a baby develops during pregnancy, problems with the spine can be linked to problems with other organs – for example, the kidneys.
Syndromic scoliosis
Scoliosis can be part of a recognised syndrome (a condition with a group of common characteristics). People with Down syndrome often have musculoskeletal problems which can include scoliosis. Marfan syndrome affects the body’s connective tissues and is likely to include scoliosis too.
Neuromuscular scoliosis
This type of scoliosis is caused by conditions that affect the nerves or muscles in your back. Such conditions include cerebral palsy. It's often worse if you can’t walk easily or at all. If the curve continues to get worse, you’ll probably need scoliosis surgery.
Postural scoliosis
This is a type of scoliosis where you look as though you have a round back when you stand, but when you lie face down or on your back, this disappears. Postural scoliosis is most common in girls. It won’t get any worse and will get better on its own so you don’t need any treatment.
Other causes
If you damage your spinal cord at any age, it can increase your risk of scoliosis. This may be through an injury, infection such as tuberculosis, or another health condition such as osteoporosis.Symptoms of scoliosis
If you have scoliosis, one shoulder – often your right one – may look higher than the other. Your shoulder blade or ribs may stick out more. And your middle (waist) may seem off-centre because your hips are uneven. Clothes may not fit or hang as well as they should or did before.
Scoliosis may cause lower back pain that gets worse as the curvature of your spine increases. And it may hurt more after you’ve been standing or sitting for a long time.
If you have adult degenerative scoliosis, you may have pain or pins and needles in your legs.
See your GP if you think you may have scoliosis.
Diagnosis of scoliosis
Your GP will ask about your medical history and your symptoms, and they’ll examine you. If you’re young, they’ll ask your parents if you’ve had any growth spurts.
If your GP thinks you have scoliosis, they may refer you to an orthopaedic specialist doctor. This is a doctor who specialises in identifying and treating bone conditions. If you have a child who may have scoliosis, your GP will refer them to a paediatric orthopaedic specialist.
The orthopaedic specialist will ask you to do a test called Adams’s forward bend test. You bend forwards from your waist. Bending your back in this way shows if your shoulders, ribs, hips, and waist are level or if your ribs are more prominent on one side. Your specialist may use an instrument called a scoliometer, to measure the curvature of your back.
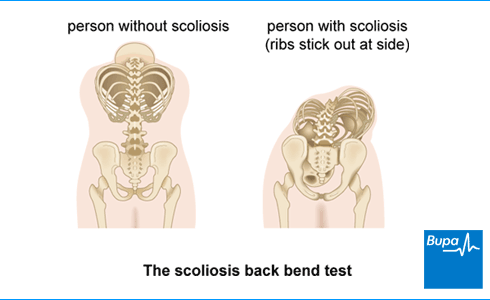
The orthopaedic specialist may arrange further tests, including:
- X-rays
- an MRI (magnetic resonance imaging) scan – particularly if you’ve had muscle weakness or changes in sensation
These tests can help to identify the cause of a curved spine and the angle of the curve.
Treatment of scoliosis
Treatment of scoliosis will depend on:
- your age
- how severe the curve in your spine is
- if it’s likely to get worse
- how it affects you.
In many younger people, scoliosis gets better on its own and they never need treatment.
If you do need scoliosis treatment, the main aims are:
- to slow or stop the curve progressing
- to relieve or prevent symptoms and complications.
Bracing
A back brace can help children that are still growing. Braces are usually used for moderately severe scoliosis. A brace can stop the curve getting worse while the spine develops. It may also help to reduce the curve, particularly when combined with exercises for scoliosis.
Braces are made specifically to fit and can be either rigid or flexible. Children can get new braces as they grow.
You may need to wear the brace every day for up to 23 hours until you stop growing. This can be difficult, particularly for children. But it’s more likely to help if you stick with it.
Casting
In babies and very young children, your specialist may suggest a plaster cast rather than a brace. This can help guide your child’s spine into a more normal position as they grow. They cover the upper body from the armpits to the hips. There’s a hole that allows the chest and stomach to expand so your child can breathe properly. The plaster cast is put on while your child is under general anaesthesia. It will need to be changed every three months as your child grows and their spine changes shape.
Other scoliosis treatments
Regular exercise is usually part of scoliosis treatment because it improves core strength and fitness. This will help to keep your back and tummy (abdominal) muscles strong enough to support your spine. Your specialist doctor may refer you to have physiotherapy before you start any new sports or exercise.
Specialist physiotherapy exercises are recommended by physios as part of treatment for mild and moderate scoliosis, including during treatment with a brace. Exercises can also help with breathing difficulties related to scoliosis.
You may decide to try complementary therapies alongside other scoliosis treatment. Therapies such as Pilates and the Alexander technique can’t cure your scoliosis but may ease pain and improve your posture, mobility and balance. Talk to your doctor first about what’s right for you. Ideally, make sure you have a specialist instructor or physio – for example, one who teaches Pilates as well. Your curve may make it hard to do some of the exercises and you should stop if it hurts. Always find a qualified practitioner, preferably one who specialises in scoliosis.
If pain from adult scoliosis is having an impact on your daily life, combined local anaesthesia and steroid injections into joints and nerves in your back may help.
Surgery
Your doctor may recommend scoliosis surgery, which can stop your spine curving and reduce related problems. Whether or not it’s an option for you will depend on how bad the curve in your spine is, and your age. A spine surgeon or an orthopaedic surgeon (a doctor who specialises in bone surgery) will operate on you.
The most common type of scoliosis surgery is called posterior instrumented correction and spinal fusion. In this procedure, your surgeon will connect metal implants and rods to bones in your spine (vertebrae) to correct the curve.
For children and adolescents, surgeons use growth rods, which are extended every six months as you grow. Once you’re fully grown, your surgeon will usually remove the rods and you’ll have a spinal fusion operation.
In older people with degenerative scoliosis, an operation to remove bone can free trapped nerves and relieve pain. This is called decompression. It’s sometimes combined with spinal fusion.
Physiotherapy services
Our evidence-based physiotherapy services are designed to address a wide range of musculoskeletal conditions, promote recovery, and enhance overall quality of life. Our physiotherapists are specialised in treating orthopaedic, rheumatological, musculoskeletal conditions and sports-related injury by using tools including education and advice, pain management strategies, exercise therapy and manual therapy techniques.
To book or to make an enquiry, call us on 0345 850 8399
Complications of scoliosis
Complications of scoliosis include the following.
- You may get a hiatus hernia or other digestive problems because of the position of your stomach has changed due to the position of your spine.
- In adults, scoliosis can cause problems walking.
- Children may get back pain or leg pain. This is because imbalance in the spine has compressed a nerve.
- If the curve of your spine restricts your lungs, it can cause breathing difficulties. This can happen to both adults and children, although it’s very rare in adolescent-onset scoliosis.
If you get scoliosis treatment early enough, you shouldn’t get these complications.
Prevention of scoliosis
You can’t prevent scoliosis but getting an early diagnosis and treatment may stop it from getting worse or even help to correct it.
There’s currently no screening programme for scoliosis in the UK. But the chances of developing scoliosis without yourself, family or friends noticing are very small. People usually spot it in themselves or in their children and see their GP. There’s no evidence that treating any earlier than that would be helpful. Doctors are also concerned that screening could lead to children having X-rays that they don’t need.
If you, or your child, is examined by a doctor for other reasons, they may detect early signs of scoliosis. Especially if you’ve already been diagnosed with a syndrome or condition linked to scoliosis.
Living with scoliosis
How scoliosis affects your daily life will depend on the severity of the curve of your spine and the treatment you have.
Poor posture can cause pain and muscle weakness and change the way you move. It can be difficult to have good posture if you have scoliosis. You may find you bend your knees and tilt your pelvis back to avoid leaning forwards or sideways. Instead, try to spread your weight evenly. Keep your neck straight and try not to tilt your pelvis. Keep your hips as level as you can. It may help to look in a mirror to check your posture, or ask your family for help.
Scoliosis can also affect your body image and confidence. See our section on other helpful websites for advice and support groups. It may help to share experiences with people going through the same thing.
You may be able to correct scoliosis with surgery. But before you consider this, there are treatments that can help to slow or stop the curve in your spine progressing. Treatment can also relieve or prevent scoliosis symptoms and complications. Most people with scoliosis don’t need treatment because the curve may stop naturally, especially in young children.
For more information, see our section on treatment of scoliosis.
There are a number of scoliosis symptoms that can vary depending on the type of scoliosis you have. But three major symptoms of scoliosis are the following.
- One shoulder, usually your right one – may look higher than the other, and it may stick out more.
- Your waist may seem off-centre because your hips are uneven.
- Lower back pain.
For more information, see our section on symptoms of scoliosis.
If you don’t get treatment for scoliosis, it may get worse. The main aims of scoliosis treatment are to slow or stop the curve progressing and to relieve or prevent symptoms and complications. Complications of scoliosis include breathing problems, if the curve of your spine restricts your lungs.
For more information, see our section on complications of scoliosis.
How scoliosis affects your daily life will depend on the severity of the curve of your spine and the treatment you have. Treatment may slow or stop the curve in your spine progressing, and relieve or prevent symptoms and complications.
Osteoporosis
Physiotherapy
Benefits of exercise
Not only does regular exercise help you manage your weight and reduce your risk of developing diseases, it can help prevent and treat mental health problems
Steroid joint injections
If you have a painful joint from an injury or arthritis, for example, your doctor may offer you a joint injection of a corticosteroid (steroid) medicine.
Back surgery
Back surgery is recommended as a treatment for back pain in certain circumstances. Find out more about the types of surgery for back pain including complications and recovery afterwards.
Did our Scoliosis information help you?
We’d love to hear what you think.∧ Our short survey takes just a few minutes to complete and helps us to keep improving our health information.
∧ The health information on this page is intended for informational purposes only. We do not endorse any commercial products, or include Bupa's fees for treatments and/or services. For more information about prices visit: www.bupa.co.uk/health/payg
This information was published by Bupa's Health Content Team and is based on reputable sources of medical evidence. It has been reviewed by appropriate medical or clinical professionals and deemed accurate on the date of review. Photos are only for illustrative purposes and do not reflect every presentation of a condition.
Any information about a treatment or procedure is generic, and does not necessarily describe that treatment or procedure as delivered by Bupa or its associated providers.
The information contained on this page and in any third party websites referred to on this page is not intended nor implied to be a substitute for professional medical advice nor is it intended to be for medical diagnosis or treatment. Third party websites are not owned or controlled by Bupa and any individual may be able to access and post messages on them. Bupa is not responsible for the content or availability of these third party websites. We do not accept advertising on this page.
- Minimally invasive fusionless posterior-approach surgery to correct idiopathic scoliosis in children and young people. The condition, current treatments and procedure. National Institute for Health and Care Excellence (NICE). www.nice.org.uk, published 22 June 2023
- Scoliosis. Paediatric Musculoskeletal Matters International. www.pmmonline.org, accessed 5 September 2024
- Adolescent idiopathic scoliosis. BMJ Best Practice. bestpractice.bmj.com, last reviewed 5 August 2024
- Menger RP, Sin AH. Adolescent idiopathic scoliosis. StatPearls Publishing. www.ncbi.nlm.nih.gov/books, last updated January 2024
- Scoliosis in children and teens. National Institute of Arthritis and Musculoskeletal and Skin Diseases. www.niams.nih.gov, last reviewed July 2023
- Scoliosis overview. British Scoliosis Society. britscoliosis.org.uk, accessed 5 September 2024
- Scoliosis. Scoliosis Research Society. www.srs.org, accessed 24 October 2024
- Infantile scoliosis. Medscape. emedicine.medscape.com, updated 13 October 2023
- What is adult degenerative scoliosis? British Scoliosis Society. britscoliosis.org.uk, accessed 5 September 2024
- Congenital scoliosis. Scoliosis Support and Research. ssr.org.uk, accessed 5 September 2024
- Lefever D, Menger RP. Infantile and juvenile scoliosis. StatPearls Publishing. www.ncbi.nlm.nih.gov/books, last updated January 2024
- Down syndrome clinical presentation. Medscape. emedicine.medscape.com, updated 21 April 2022
- Marfan syndrome (MFS). Medscape. emedicine.medscape.com, updated 1 July 2024
- Neuromuscular scoliosis. British Scoliosis Society. britscoliosis.org.uk, accessed 5 September 2024
- Scoliosis and kyphosis. Patient. patient.info, last edited 23 August 2021
- Idiopathic scoliosis. MSD Manuals. msdmanuals.com, reviewed/revised November 2022
- Early onset scoliosis. Scoliosis Support and Research. ssr.org.uk, accessed 5 September 2024
- Scoliosis back bracing. Scoliosis Support and Research. ssr.org.uk, accessed 5 September 2024
- What is early onset scoliosis? British Scoliosis Society. britscoliosis.org.uk, accessed 5 September 2024
- Seleviciene V, Cesnaviciute A, Strukcinskiene B, et al. Physiotherapeutic scoliosis-specific exercise methodologies used for conservative treatment of adolescent idiopathic scoliosis, and their effectiveness: An extended literature review of current research and practice. Int J Environ Res Public Health 2022; 19(15):9240. doi: 10.3390/ijerph19159240
- Amăricăi E, Suciu O, Onofrei RR, et al. Respiratory function, functional capacity, and physical activity behaviours in children and adolescents with scoliosis. J Int Med Res 2020; 48(4):300060519895093. doi: 10.1177/0300060519895093
- Complementary therapies. Scoliosis Support and Research. ssr.org.uk, accessed 5 September 2024
- What is adolescent idiopathic scoliosis? British Scoliosis Society. britscoliosis.org.uk, accessed 5 September 2024
- Hiatus hernia. Patient. patient.info, last edited 16 August 2024
- Musculoskeletal problems. Oxford Handbook of General Practice. Oxford Academic. academic.oup.com, published online June 2020
- Child screening programme. Scoliosis. UK National Screening Committee. view-health-screening-recommendations.service.gov.uk, accessed reviewed 2021
- UK National Screening Committee (UK NSC). Screening for adolescent idiopathic scoliosis in children. UK National Screening Committee. view-health-screening-recommendations.service.gov.uk, reviewed 5 March 2021
- Posture and positioning. Scoliosis Support and Research. ssr.org.uk, accessed 5 September 2024
- Scoliosis. Changing Faces. www.changingfaces.org.uk, accessed 6 September 2024
- Rachael Mayfield-Blake, Freelance Health Editor



