Ultrasound
- Dr Paul Crowe, Consultant Interventional Radiologist
An ultrasound is a type of scan that uses sound waves to produce images of the inside of your body. It can pick up changes in your organs, tissues, vessels, and joints. This may help in diagnosing health problems. Ultrasound scans are also used in certain procedures, and during pregnancy.
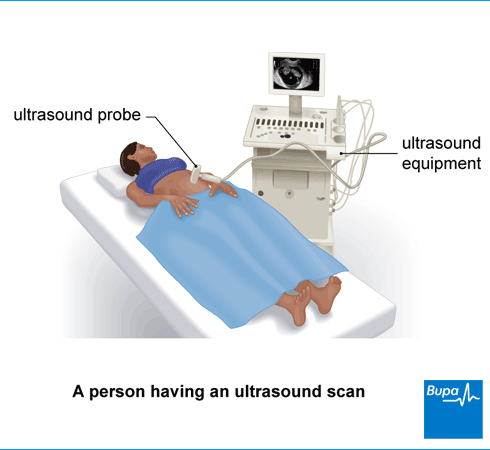
About ultrasound
An ultrasound machine consists of a small hand-held scanner (or ‘probe’) with a transducer that sends out sound waves. The sound waves are a high frequency that you can’t hear. The sound waves bounce off the organs or tissues inside your body and are picked up again by the probe.
The probe is linked to a computer that creates real-time images from the reflected sound waves. The images are displayed on a monitor in various shades of grey. The pictures are constantly updated, which means the scan can show movement. The pictures can be captured, saved, and shared with you.
As well as computer-based ultrasound machines there are also hand-held ones. These are much smaller and easier to transport.
Several different types of health professional may carry out ultrasound scans. These include sonographers (specialists in ultrasound) and radiologists (doctors specialising in imaging methods).
Ultrasound uses
You can have an ultrasound on different parts of your body and for many different reasons. These include:
- muscles and joints to check for injury or health conditions such as arthritis
- your abdomen to check the health of organs such as your liver, gallbladder, kidneys, and pancreas
- reproductive organs such as your womb and ovaries or prostate and testes
- your breasts, to check lumps, alongside other tests such as mammograms and biopsies
- lumps under your skin, anywhere around your body
- blood vessels – to check for conditions like deep vein thrombosis and varicose veins, or to check arteries to assess risk of stroke
You might need an ultrasound scan to check to help diagnose cancer or check for other health conditions. It can check the health of your baby when you’re pregnant.
Ultrasound is also used to help doctors and surgeons perform certain procedures. These include biopsy, which involves taking a sample of cells using a small needle, and steroid joint injections. Ultrasound helps your doctor to guide the needle to the right place.
The health professional referring you will explain why they are recommending you go for an ultrasound scan. Make sure to ask any questions you might have, because you’ll need to give your consent when you go for the scan.
Types of ultrasound
There are three main types of ultrasound: external, internal, and endoscopic.
- In an external ultrasound, the ultrasound practitioner will move the ultrasound probe over your skin.
- In an internal ultrasound, the ultrasound practitioner places the probe inside your body to take the scan. This may be in your vagina (transvaginal ultrasound) to check your womb and ovaries. Or the probe may be placed in your back passage to check your prostate, if you have one (transrectal ultrasound). It can also be used to take images inside your back passage.
- An endoscopic ultrasound is a combination of an endoscopy (gastroscopy) and an ultrasound scan. The practitioner uses a probe attached to a long, thin, flexible tube (an endoscope) to look further inside your body. The probe is passed into your mouth and down your food pipe (oesophagus) to check for problems in your digestive system.
There are some types of ultrasound that use special techniques. These include the following.
- Echocardiogram. This is an ultrasound of your heart. An echocardiogram is able to produce real-time images of blood flowing through your heart
- Doppler (or Duplex) ultrasound. This is a type of ultrasound that can monitor blood flow in your blood vessels. It can show how fast and in which direction your blood is flowing. This can help detect blood clots or narrowed blood vessels.
- 3D ultrasound. Standard ultrasound creates 2D (flat) images. But newer technology is also able to produce 3D ultrasound images. This may make it easier to see any problems.
- Elastography. This is a special type of ultrasound technique that can measure the stiffness of organs inside your body. It’s most commonly used to check if you have liver fibrosis (scarring). Fibrosis can be due to alcohol-related liver disease, non-alcoholic fatty liver disease, and hepatitis.
- Contrast-enhanced ultrasound. This is a type of ultrasound that uses contrast agent (dye) to show up your vessels or organs more clearly. Your doctor or sonographer injects very small gas bubbles with the contrast agent into your vein before the procedure.
Preparation for ultrasound
Whether or not you need to do anything to prepare for your ultrasound depends on the type of ultrasound you’re going to have. For some types of ultrasound, you may be asked to follow instructions about eating or drinking before your ultrasound. This is to make it easier for the practitioner to create clear images.
- If you’re having a scan of your womb, bladder, or kidneys, you may need to drink something before so you have a full bladder. Sometimes you may then be asked to go for a pee, so the ultrasound can be repeated when you have an empty bladder.
- If you’re having a scan of your gallbladder or pancreas, you may be asked to stop eating for about six hours before the scan.
- If you’re having a transrectal ultrasound, you may be asked to make sure your bowel is empty before your appointment.
- If you’re having an endoscopic ultrasound, you’ll usually need to stop eating at least six hours beforehand, so your bowel is clear. You can usually carry on drinking for two hours before the test. You may need to have more preparation as part of having a gastroscopy.
Ultrasound procedure
An ultrasound appointment usually takes at least 20 minutes. This may be longer or shorter, depending on why you’re having it. The person doing your scan will explain the procedure to you and check you’re happy to go ahead.
If necessary, you might be asked to remove clothing or to change into a hospital gown. This depends on the part of your body you’re having scanned.
If you’re having an abdominal ultrasound, you’ll usually need to lie on your back on a couch. Your ultrasound practitioner will put some gel on your skin on the area they’re going to examine. This may feel cold. The gel will help the probe make secure contact with your body and also help to transmit the soundwaves between your body and the probe.
The practitioner will hold the probe firmly against your skin and move it over the surface. They may ask you to take some deep breaths or to move into different positions so they can get the best possible images.
An ultrasound isn’t painful, but you might feel some slight discomfort as the probe is pressed against you, particularly if the area is tender. Tell the person doing your scan if you feel uncomfortable.
After an ultrasound, your practitioner will usually wipe the gel off your skin. If any is left, it won’t stain your clothing. You’ll be able to wash it off with soap and water when you get home.
Transvaginal ultrasound
If you’re having a transvaginal ultrasound, the ultrasound practitioner will ask you to lie on your back with your knees raised and legs apart. If this is difficult for you, you may be able to lie on your side with your knees pulled up to your chest instead.
The practitioner inserts a small, thin, ultrasound probe (similar in size to a tampon) into your vagina. They’ll put a protective cover over the probe, and it will have some gel on it. It’s important to tell your hospital if you have a latex allergy so they can use a suitable cover.
The test may be a bit uncomfortable, but it shouldn’t be painful.
Transrectal ultrasound
If you’re having a transrectal ultrasound, your practitioner will ask you to lie on your left side with your knees pulled up towards your chest. Your practitioner will insert a small, thin ultrasound probe into your back passage. The probe will have a protective cover and lubricating gel on it. If you have a latex allergy, tell the practitioner so they can use a suitable cover.
A transrectal ultrasound may feel a bit uncomfortable but it shouldn't be painful.
Endoscopic ultrasound
You’ll usually have a sedative for an endoscopic ultrasound. This will make you feel relaxed and sleepy, but you’ll still be awake.
The health professional performing the test may spray some local anaesthetic on your throat to numb it. They’ll then pass the endoscope through your mouth and guide it towards the area of your body that’s being checked. You may need to swallow as the tube goes down. Once the practitioner has the images they need, they’ll gently remove the endoscope.
Aftercare for ultrasound
After an ultrasound, you can usually go straight home or continue with your usual activities.
If you’ve had a sedative, you may need to rest for a while until the effects have worn off. Ask a friend or family member to take you home by car or taxi – ideally not public transport. The effects of sedation can last up to 24 hours so ask them to stay overnight to look after you. Don’t drive, drink alcohol, operate machinery or make any important decisions during this time. Your hospital will give you more information about having a sedative before your scan.
During an endoscopic ultrasound, your doctor may have used a spray to numb your throat. It’s best to wait about an hour for this to wear off before you eat or drink anything. You might have a sore throat for up to 24 hours.
Getting your ultrasound results
Your ultrasound practitioner may be able to discuss the results with you during or straight after your scan. This isn’t always possible though. The results will always be sent to the health professional who referred you for the scan. They can discuss them with you if you didn’t get results on the day. In that case, ask how long it should take to get the results.
Risks of ultrasound
An ultrasound is considered safe because it doesn’t use any radiation. So, unlike scans such as X-rays and CT scans, which do use radiation, there aren’t any of the associated risks. Even so, ultrasound scans should only be done for clear medical reasons. You shouldn’t have an ultrasound scan unnecessarily.
Alternatives to ultrasound
Alternatives to ultrasound imaging depend on what you’re having it for. It will also depend on what part of your body is being looked at and your individual circumstances. Alternative scans may include:
You may have ultrasound as well as these other scans. Your doctor will talk you through which type of scan is most suitable for you.
GP Subscriptions – Access a GP whenever you need one for less than £20 per month
You can’t predict when you might want to see a GP, but you can be ready for when you do. Our GP subscriptions are available to anyone over 18 and give you peace of mind, with 15-minute appointments when it suits you at no extra cost.
You may have an ultrasound to help diagnose a health condition or injury or to check for problems as part of a screening test. The scan can pick up changes in your organs, tissues, blood vessels or joints. You may also have an ultrasound as part of a medical procedure or to check how a baby is developing during pregnancy. See our section on ultrasound uses to find out more.
There are three main ways to have an ultrasound. These include:
- an external ultrasound, where an ultrasound probe is moved over the surface of your skin
- an internal ultrasound, where a probe is inserted into your vagina or back passage
- an endoscopic ultrasound, where a probe attached to a long, flexible tube called an endoscope, is used to look inside your body
Read more on these types in our section on types of ultrasound.
Sometimes the health professional carrying out your scan may be able to discuss the results straight away. But this doesn’t always happen. Sometimes they will send a report to the doctor or health professional who referred you for the test. You should ask how long it will take for the results to be sent through. Read more in our section on aftercare for ultrasound.
Antenatal care
Did our Ultrasound information help you?
We’d love to hear what you think.∧ Our short survey takes just a few minutes to complete and helps us to keep improving our health information.
∧ The health information on this page is intended for informational purposes only. We do not endorse any commercial products, or include Bupa's fees for treatments and/or services. For more information about prices visit: www.bupa.co.uk/health/payg
This information was published by Bupa's Health Content Team and is based on reputable sources of medical evidence. It has been reviewed by appropriate medical or clinical professionals and deemed accurate on the date of review. Photos are only for illustrative purposes and do not reflect every presentation of a condition.
Any information about a treatment or procedure is generic, and does not necessarily describe that treatment or procedure as delivered by Bupa or its associated providers.
The information contained on this page and in any third party websites referred to on this page is not intended nor implied to be a substitute for professional medical advice nor is it intended to be for medical diagnosis or treatment. Third party websites are not owned or controlled by Bupa and any individual may be able to access and post messages on them. Bupa is not responsible for the content or availability of these third party websites. We do not accept advertising on this page.
- Non-obstetric ultrasound scanning. Patient. patient.info, last edited 23 December 2021
- Guidelines for professional ultrasound practice. Society of Radiographers and British Medical Ultrasound Society. Sixth edition. www.bmus.org, published December 2021
- Ultrasonography. MSD Manuals. msdmanuals.com, last review/revision April 2021
- Upper and lower limb venous duplex ultrasound examination for the assessment of deep vein thrombosis (DVT). The Society for Vascular Technology of Great Britain and Ireland. www.svtgbi.org.uk, reviewed March 2021
- Ultrasound scan. Cancer Research UK. www.cancerresearchuk.org, last reviewed 7 November 2022
- Echocardiography. MSD Manuals. msdmanuals.com, last review/revision July 2021
- Iommi D, Hummel J, Figl ML. Evaluation of 3D ultrasound for image guidance. PLoS One 2020; 26;15(3):e0229441. doi: 10.1371/journal.pone.0229441
- Mahfouz MR, Abdel Fatah EE, Johnson JM, et al. A novel approach to 3D bone creation in minutes: 3D ultrasound. Bone Joint J 2021; 103–B(6 Supple A):81–6. doi: 10.1302/0301-620X.103B6.BJJ-2020-2455.R1
- Kurzweil A, Martin J. Transabdominal ultrasound. StatPearls Publishing. www.ncbi.nlm.nih.gov, last updated 8 August 2021
- Gastroscopy. Cancer Research UK. www.cancerresearchuk.org, last reviewed 9 September 2022
- Nahlawi S, Gari N. Sonography transvaginal assessment, protocols, and interpretation. StatPearls Publishing. www.ncbi.nlm.nih.gov, last updated 16 September 2022
- Wonski S, Carter KR. Sonography endorectal prostate assessment, protocols, and interpretation. StatPearls Publishing. www.ncbi.nlm.nih.gov, last updated 21 August 2022
- Sedation explained. Royal College of Anaesthetists. rcoa.ac.uk, published June 2021
- Endoscopic ultrasound (EUS) for oesophageal cancer. Cancer Research UK. www.cancerresearchuk.org, last reviewed 20 September 2019
- Diagnostic imaging and scans. Patient. patient.info, last edited 8 November 2018
- Pippa Coulter, Freelance Health Editor



