Cervical artery dissection
- Dr David Paling, Consultant Neurologist
- Liz Woolf, Freelance Health Editor
Cervical artery dissection means you have a tear in the wall of a large blood vessel (artery) in your neck. This can cause blood clots in your arteries, which can affect the blood supply to your brain. Cervical artery dissection is one of the most common causes of stroke in people under 50.
About cervical artery dissection
Arteries carry blood from your heart to the rest of your body. You have two pairs of large arteries on each side of your neck, which carry blood to your brain. The carotid arteries supply blood to each side of the front of your brain. The vertebral arteries supply the back of the brain. Together, these arteries are known as cervical arteries. You may hear cervical artery dissection called vertebral artery dissection or carotid artery dissection, depending on where the tear is.
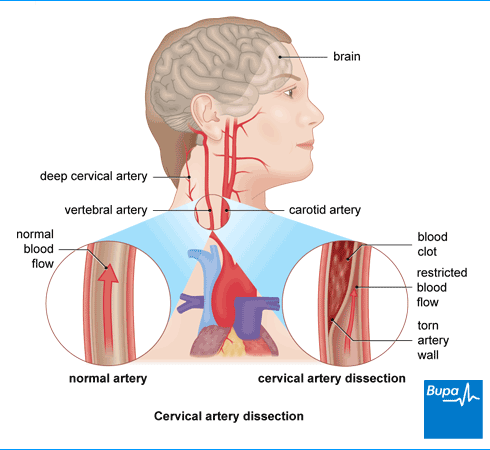
Cervical artery dissection means that the wall of one of these arteries has torn inside. This is more likely to happen in your carotid arteries than in your vertebral arteries. Once the wall has torn, blood can stick to it and form a clot. This can block the artery around the tear. Or, if all or part of the clot breaks off, it can block the artery further up.
If a blood clot blocks an artery, it can cause a stroke. This affects the blood supply to your brain and can damage brain cells. The symptoms of a stroke depend on where it happens in your brain. It can affect your movement, sensation, speech, sight and thinking.
Causes of cervical artery dissection
The two main potential cervical artery dissection causes are:
- an injury or strain
- a health condition that may weaken your blood vessels
However, usually cervical artery dissection happens without an obvious injury or underlying health condition.
Injuries
Cervical artery dissection can happen after a sudden movement or injury to your neck, such as:
- a high-impact injury from an accident such as a car crash
- a minor neck injury from sports like running, yoga or volleyball
- neck strain from activities such as painting a ceiling
- coughing, blowing your nose or sneezing
Health conditions
Cervical artery dissection may happen with some underlying health conditions. It has been linked to:
- inherited conditions – for example, Ehlers–Danlos syndrome and Marfan syndrome
- high blood pressure
- a problem with your blood vessels – for example, a condition called fibromuscular dysplasia
Symptoms of cervical artery dissection
It may be difficult to know if you have cervical artery dissection. Symptoms may be vague and can vary from person to person. They depend on how badly your artery is affected and whether you have a stroke afterwards. Your symptoms will also depend on whether you tear a carotid or a vertebral artery.
Carotid artery dissection symptoms
Some of the main symptoms of carotid artery dissection are:
- a really bad headache
- neck pain, usually on one side
- pain on one side of your face
- pulsating tinnitus – a rhythmic noise in your ears, beating in time to your heart
- sight problems – completely losing sight temporarily or seeing shimmering lights
- a painful drooping eyelid
Vertebral artery dissection symptoms
Some symptoms of vertebral artery dissection are similar to those above. You may have a bad headache and pain in the nape of your neck. You may also have:
- vertigo (a feeling of moving or spinning when you’re not)
- numbness in your face
- a hoarse voice
- difficulty speaking or swallowing
- not being able to feel pain, heat or cold on one side of your body
- loss of taste
- hiccups
- feeling or being sick
- double-vision
- hearing loss on one side
- loss of balance
Stroke symptoms
A stroke after cervical artery dissection can cause other symptoms. Stroke symptoms depend on the area of the brain involved, but may include:
- numbness and weakness on one side of your body
- not being able to move one side of your body
- difficulties with speech
- loss of sight in one eye
- confusion
- numbness and drooping on one side of your face
- problems with coordination
Some of the symptoms above can be caused by other, less serious, health problems. But you should seek emergency help if your symptoms come on suddenly. Or if you develop symptoms after you’ve hurt your neck.
Looking for prompt access to quality care?
With our health insurance, if you develop new conditions in the future, you could get the help you need as quickly as possible, from treatment through to aftercare.
To get a quote or to make an enquiry, call us on 0800 600 500∧
Diagnosis of cervical artery dissection
Your doctor will ask about your symptoms and examine you. Tell them if you’ve had any recent injuries, or have taken part in any activities that could have torn one of your cervical arteries.
You may have one or more of the following tests to diagnose a cervical artery dissection.
- An MRI (magnetic resonance imaging) scan or a CT (computerised tomography) scan. These create detailed images of your head and neck. The scan usually also involves an angiogram, where the doctor looks closely at the blood vessels in the area. To have this done, you may have an injection of a medical dye into your arteries. This helps your doctor to see blood vessels in more detail.
- An ultrasound scan of your arteries. This scan uses sound waves to produce an image of your blood vessels.
Treatment of cervical artery dissection
Cervical artery dissection treatment can vary. The treatment you need will depend on:
- where the tear is
- how quickly you can get treatment
- if you have any complications
The aim of treatment is to prevent complications, such as a stroke, while your artery heals. This usually takes about three to six months. Your doctor will monitor you closely, checking for possible stroke symptoms. They’ll also check for any side-effects from the medicines used to prevent blood clots.
Medicines for cervical artery dissection
If you have stroke symptoms, you may be able to have a medicine to break up the blood clot. You have to be treated within four-and-a-half hours of your symptoms starting. This treatment is called thrombolysis. Your doctor will inject a medicine called a fibrinolytic into your vein. This breaks up blood clots, but will only help in the first few hours after a stroke.
If the clot is large, your doctor may arrange additional tests to see if you can have a thrombectomy after thrombolysis. While you are sedated, the doctor puts a tube into an artery in your groin. They can then thread the tube up to where the clot is and pull it out. They may also put in a tube (a stent) to keep the artery open. You can have this done up to six hours after a stroke, although sometimes it can be done later.
Longer term, your doctor will probably suggest that you take medicines to prevent blood clots. The two main types are:
- antiplatelet medicines, such as aspirin or clopidogrel
- anticoagulants, such as heparin and warfarin
When taking warfarin, you will need regular blood tests to monitor your blood clotting and make sure it’s working as it should.
How long you need to take these medicines for can vary – ask your doctor for advice.
Surgery for cervical artery dissection
Medicines usually work well, so doctors only consider surgery if medicines aren’t working for you. Your doctor may suggest putting a tube into your artery. This ‘stent’ holds it open, allowing blood to flow through. The procedure is called angioplasty and stenting. It’s done the same way as the thrombectomy described above, with a tube threaded through your blood vessels to reach the clot.
Other surgical procedures are done much more rarely. Ask your doctor for information about these.
Complications of cervical artery dissection
If you have a cervical artery dissection, you may have complications. Some people get headaches afterwards, which can last on and off for years. Others go on to have a stroke. Sometimes strokes are relatively minor. But they may also cause severe disability and be life-threatening.
If you have any head and neck pain after cervical artery dissection, it usually settles after a few weeks. But some people do continue to get headaches or neck pain afterwards from time to time.
There’s a risk of having another tear in the wall of one of your cervical arteries. The chances of this happening are low. It happens to about one in 100 people a year (1 percent)
Some people have cervical artery dissection without any obvious reason why. But it may be caused by an injury, a neck strain, or a health condition that weakens your blood vessels. For more information see our causes of cervical artery dissection section.
Cervical artery dissection isn’t very common – it affects around four people in every 100,000. But it’s a common cause of stroke in otherwise healthy young people. It causes around one in four strokes in young adults and is a frequent cause of stroke in people under 50.
Symptoms of carotid artery dissection include a bad headache and face and neck pain. Some people have problems with sight. Other symptoms include migraines and a painful, drooping eyelid. For more information, see our symptoms of cervical artery dissection section.
Symptoms of vertebral artery dissection include facial pain and numbness. You might have difficulty speaking or swallowing and have a hoarse voice. You may also have double-vision and problems with balance. For more information, see our symptoms of cervical artery dissection section.
Other helpful websites
Discover other helpful health information websites.
Did our Cervical artery dissection information help you?
We’d love to hear what you think.∧ Our short survey takes just a few minutes to complete and helps us to keep improving our health information.
∧ The health information on this page is intended for informational purposes only. We do not endorse any commercial products, or include Bupa's fees for treatments and/or services. For more information about prices visit: www.bupa.co.uk/health/payg
This information was published by Bupa's Health Content Team and is based on reputable sources of medical evidence. It has been reviewed by appropriate medical or clinical professionals and deemed accurate on the date of review. Photos are only for illustrative purposes and do not reflect every presentation of a condition.
Any information about a treatment or procedure is generic, and does not necessarily describe that treatment or procedure as delivered by Bupa or its associated providers.
The information contained on this page and in any third party websites referred to on this page is not intended nor implied to be a substitute for professional medical advice nor is it intended to be for medical diagnosis or treatment. Third party websites are not owned or controlled by Bupa and any individual may be able to access and post messages on them. Bupa is not responsible for the content or availability of these third party websites. We do not accept advertising on this page.
- Carotid Artery Dissection. Medscape. emedicine.medscape.com, last updated February 2019
- Cervical Artery Dissection. Royal College Emergency Medicine. rcemlearning.co.uk, published October 2020
- Cardiovascular System Anatomy. Medscape. emedicine.medscape.com, last updated 20 August 2014
- Hynes N, Kavanagh EP, Sultan S, et al. Surgical and radiological interventions for treating symptomatic extracranial cervical artery dissection. Cochrane Database of Systematic Reviews, Issue 2. Art. No.: CD013118. DOI: 10.1002/14651858.CD013118.pub2, published February 2021
- Stroke and tia. Nice Clinical Knowledge Summaries. cks.nice.org.uk, last revised August 2020
- Ischaemic stroke. BMJ Best Practice. bestpractice.bmj.com, last reviewed October 2023
- Keser Z, Chiang C-C, Benson J, et al. Cervical artery dissections: Etiopathogenesis and management. Vasc Health Risk Manage 2022; 18:685–70, published September 2022
- Britt TB, Agarwal S. Vertebral artery dissection. National Library of Medicine: StatPearls Publishing, last updated March 2023
- Vertebral Artery Dissection. Medscape. emedicine.medscape.com, last updated February 2019
- Mitra A, Azad HA, Prasad N, et al. Chiropractic associated vertebral artery dissection: An analysis of 34 patients amongst a cohort of 310. Clin Neurol Neurosurg, 2021; 206:106665, published July 2021
- Carotid Artery Dissection Clinical Presentation. Medscape. emedicine.medscape.com, last updated February 2019
- Vertebral Artery Dissection Clinical Presentation. Medscape. emedicine.medscape.com, last updated February 2019
- Stroke and TIA. Nice Clinical Knowledge Summaries. cks.nice.org.uk, last revised October 2023
- Assessment of neck pain. BMJ Best Practice. bestpractice.bmj.com, last reviewed October 2023
- Carotid Artery Dissection Workup. Medscape. emedicine.medscape.com, last updated February 2019
- Vertebral Artery Dissection Workup. Medscape. emedicine.medscape.com, last updated February 2019
- Carotid Artery Dissection Treatment and Management. Medscape. emedicine.medscape.com, last updated February 2019
- Vertebral Artery Dissection Treatment and Management. Medscape. emedicine.medscape.com, last updated February 2019
- Dissection Syndromes Medication. Medscape. emedicine.medscape.com, last updated November 2018
- Dissection Syndromes Treatment and Management. Medscape. emedicine.medscape.com, last updated November 2018
- Stroke. Nice British National Formulary. bnf.nice.org.uk, accessed November 2023
- Alteplase. Nice British National Formulary. bnf.nice.org.uk, accessed November 2023
- Thrombectomy. Stroke Association. stroke.org.uk, accessed November 2023
- Angioplasty and stent placement – carotid artery. Medline Plus. medlineplus.gov, last reviewed January 2023
- Goodfriend SD, Tadi P, Koury R. Carotid artery dissection. National Library of Medicine: StatPearls Publishing. ncbi.nlm.nih.gov, last updated December 2019



