Lung cancer
- Dr James Wilson, Consultant Clinical Oncologist
Lung cancer is the third most common cancer in the UK. It can cause a persistent cough, breathlessness, and weight loss. Most cases of lung cancer are caused by smoking.
What is lung cancer?
You may get lung cancer if cells in your lungs grow in an uncontrolled way. The cells usually form a lump (tumour).
Your lungs move oxygen from the air you breathe into your blood and remove carbon dioxide as you breathe out. They’re made up of lots of air tubes (called bronchioles) and air sacs (called alveoli).
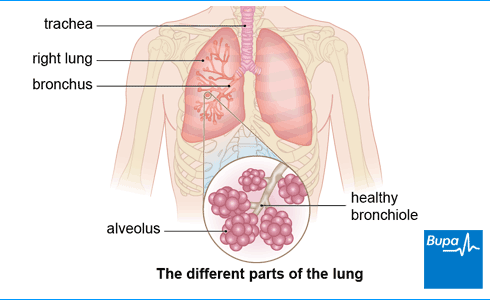
You have different types of cells in the different parts of your lungs. This means you can get different types of lung cancer.
You may have:
- primary lung cancer – when a tumour starts in your lung
- secondary lung cancer – when cancer cells have spread to your lungs through your bloodstream or immune system from cancer that started in another part of your body, such as your kidney, breast , or prostate
Over 49,000 people are diagnosed with lung cancer each year in the UK.
Types of lung cancer
The two main types of cancer that start in the lung are:
- non-small cell lung cancer (NSCLC)
- small cell lung cancer (SCLC)
These names come from how the cancer cells look under a microscope.
Non-small cell lung cancer
About 8 in every 10 primary lung cancers are NSCLC. There are three main types of NSCLC:
- adenocarcinoma
- squamous cell carcinoma
- large cell carcinoma
Adenocarcinoma mainly affects the outer part of your lungs. Around 4 in every 10 people with NSCLC have adenocarcinoma. This is related to smoking. But it’s also the type of lung cancer you’re most likely to get if you don’t smoke. It can be caused by air pollution or asbestos.
Squamous cell carcinoma affects your main airways (your bronchi). It’s usually near the centre of your lungs. Around 3 in every 10 people with NSCLC have this type of lung cancer.
Large cell carcinoma can appear in any part of your lungs, but most often in the centre of your lungs. It affects about 1 in every 10 people with NSCLC.
Small cell lung cancer
Two in 10 people with lung cancer have SCLC. SCLC can start quickly and spread to other parts of your body, often before it’s been diagnosed. SCLC is almost always caused by smoking.
Causes of lung cancer
Smoking (tobacco cigarettes) is the biggest cause of lung cancer. In the UK, it causes over 8 in every 10 lung cancers. Your risk of lung cancer is related to how much you smoke, how long you’ve been smoking and when you started smoking. Passive or second-hand smoking (breathing in other people’s smoke) is also linked to lung cancer.
You may also be more likely to get lung cancer if you:
- are exposed to asbestos
- are exposed to high levels of radon gas – a naturally occurring radioactive gas
- have had lung disease such as tuberculosis (TB) or chronic obstructive pulmonary disease (COPD) in the past
How cancer develops
Cancer explained | Watch in 1:48 minutes
In this video, we explain how, when cells divide uncontrollably, this leads to cancer.
Symptoms of lung cancer
Many people with lung cancer don’t have any symptoms at first. Sometimes, the early symptoms can be very general, such as a cough or feeling a bit out of breath. You may think these symptoms are caused by other smoking-related lung problems, such as asthma or COPD. Lung cancer is sometimes only discovered if you have a chest X-ray for some other reason.
Lung cancer symptoms can include:
- a cough that doesn’t go away (lasts longer than three weeks) or changes in some way (it may get more painful or sound different)
- coughing up blood
- shortness of breath
- pain in your chest
- losing weight for no reason
- feeling very tired
- losing your appetite
Other symptoms of lung cancer include:
- swelling of your face or neck
- a hoarse voice
- regular chest infections
You may also notice a broadening or thickening of the tips of your fingers – this is called clubbing.

If you have any of these symptoms or signs, see a GP as soon as possible.
Diagnosis of lung cancer
NHS Lung Health Checks
NHS Lung Health Checks aim to diagnose lung cancer at an early stage when the cancer is easier to treat. The service is now changing to a targeted lung cancer screening service in England.
You may be invited to an NHS Lung Health Check if:
- you live in some parts of England and Wales – this service isn’t available everywhere yet
- you’re aged 55 to 74
- you are a current or former smoker
You’ll be asked about your breathing, lifestyle, family, and medical history. If you may be at a higher risk of lung cancer, you may be offered a low-dose computer tomography (CT) scan to create a detailed picture of your lung.
Seeing your GP
If you have any symptoms, a GP will ask you about your symptoms and medical history and whether or not you smoke. If you only have a cough, they may ask you to wait and see if it gets better on its own. This is most likely to happen if you’re younger, have never smoked, or your cough started when you had a cold or flu.
If your GP thinks your symptoms could be caused by lung cancer, they’ll refer you for a chest X-ray or a scan. You may have an urgent clinic referral if you’re over 40 and you smoke or have smoked in the past.
Referral to a specialist
If your chest X-ray shows signs of lung cancer, a GP will refer you to a doctor who specialises in chest disease. Sometimes, they may refer you even if your X-ray seems normal or before you have any X-rays.
The specialist will ask you to have some tests to confirm whether or not you have lung cancer. If you do have cancer, the tests can show which type of cancer you have, how advanced it is, and if it’s spread (metastasised). This is called cancer staging.
These tests may include the following.
- A CT scan of your chest and tummy. This uses X-rays to make three-dimensional (3D) images of part of your body. It’s usually the first test you’ll have after a chest X-ray.
- A PET-CT (positron emission tomography) scan. You may be offered this type of CT scan if you have early-stage cancer. It helps doctors to see where your cancer is and if the cancer has spread.
- A bronchoscopy. This test lets your doctor look inside your lungs and take a sample of tissue (a biopsy). A bronchoscope is a narrow, tube-like, flexible telescopic camera. You’ll be given an anaesthetic spray and some medicine to make you sleepy. Or you may have a general anaesthetic and be asleep during the test. The doctor passes the bronchoscope down your windpipe into your lungs.
- A needle biopsy through the skin of your chest. This is called a percutaneous lung biopsy. Your doctor will numb your skin with a local anaesthetic then insert a fine needle. They’ll use an ultrasound or CT scan to guide the needle into the right place.
Looking for cancer cover that supports you every step of the way?
If you develop new conditions in the future, you can rest assured that our health insurance comes with full cancer cover as standard.
To get a quote or to make an enquiry, call us on 0800 600 500∧
Treatment of lung cancer
Treatment for lung cancer will depend on:
- which type of cancer you have
- the stage of the cancer
- your general health
The stage of cancer is how big it is and if it has spread. The tests you have to diagnose your cancer give some information about the stage. This information can help your doctor decide which treatment you need.
Lung cancer can be difficult to cure because it may have already spread by the time you’re diagnosed.
Non-small cell lung cancer
Non-small cell lung cancer (NSCLC) that’s at an early stage and hasn’t spread is usually treated with surgery or radiotherapy first. This may cure some types of NSCLC. Surgery may be followed by chemotherapy. If the cancer has already spread (metastasised), you may be offered treatments such as chemotherapy, radiotherapy, immunotherapy, or targeted therapy.
Small cell lung cancer (SCLC)
Small cell lung cancer (SCLC) is usually treated with chemotherapy and radiotherapy rather than with surgery.
Surgery
Your surgeon may remove a small section of lung, part of a lung, or a whole lung, depending on the size, type, and position of your cancer.
Whether or not you’re offered surgery will depend on how healthy your lungs are. If you smoke, it’s best to stop smoking before your operation because this will help you to recover better afterwards. Before surgery, your doctor may give you some advice on how to get yourself as fit as possible so you’re ready for your operation.
Non-surgical treatments
Radiotherapy uses radiation to destroy cancer cells. Your doctor will target a beam of radiation onto the area of your lung with the cancer to shrink the tumour.
Chemotherapy uses medicines to destroy cancer cells. You may have chemotherapy on its own, after surgery, or with radiotherapy. Chemotherapy is usually given as an injection or through a drip.
Targeted therapies are medicines that can block messages in your cancer cells to stop them growing and dividing. You may be offered targeted therapy if you have a particular type of NSCLC.
Immunotherapy is another type of cancer treatment. It helps your immune system to attack cancer cells. A number of immunotherapy drugs are now available to treat advanced NSCLC.
All lung cancer treatments can help to manage your cancer, but they can also cause side-effects. Your doctors and nurses will give you information about the treatments. This will help you decide which treatment is right for you and what to expect.
If it isn’t possible to cure your cancer, your treatment will aim to improve your quality of life as much as possible. Palliative care will help to relieve and manage your symptoms and support you as well as your family and friends.
Prevention of lung cancer
The most important thing you can do to reduce your risk of developing lung cancer is to stop smoking. Speak to your local pharmacist or GP about the best ways to give up smoking. Nicotine replacement therapy (such as gums or patches) can help you quit. Vaping may be an option for you to consider. But quitting completely is better for your health.
Try to avoid second-hand smoke – keep away from enclosed spaces where other people are smoking. Try to avoid exposing yourself to anything that could increase your risk of lung cancer – this includes asbestos and radiation.
There’s some evidence that eating fruit and vegetables can help to reduce your risk of getting lung cancer. So try to eat a balanced diet. Research suggests that taking vitamin supplements doesn’t seem to have any effect on the risk of lung cancer and may even be harmful.
Being more physically active may help to reduce your chance of getting several cancers.
Living with lung cancer
A lung cancer diagnosis can be distressing for you and your loved ones. An important part of cancer treatment is getting enough support to deal with the emotional aspects as well as the physical symptoms.
You should have a lung cancer clinical nurse specialist assigned to you as soon as you’ve been diagnosed. This person will coordinate your care. A range of doctors and nurses will help to support you through your treatment and help you to make decisions about the type of treatment you’d like. They can prescribe medicines and offer practical advice to deal with symptoms, such as pain, exhaustion, coughing, and depression.
Your hospital should also offer a range of helpful services, including dietitians, counsellors, complementary therapists, and benefits advisers. Voluntary groups and patient organisations, such as Macmillan nurses and Marie Curie nursing, and day centres are also available.
If you have more advanced cancer, you can get support through specialist palliative care teams – either at your local hospice or in your own home. Your doctor will discuss this with you.
Ask your cancer specialist about any new cancer treatments you see in the news. The treatments may be in the experimental stages and you might be able to join a local clinical trial. Your cancer specialist can tell you if you’re right for the trial and if the treatment being tested could be right for you. You can find out more about clinical trials happening near you on the Cancer Research UK website.
The nurses and physiotherapists in the hospital will encourage you to be up and walking a little as soon as possible after your surgery. But it’s normal to feel tired for several weeks or even months afterwards. Everyone recovers differently from surgery. So before you leave the hospital, ask your doctor or physiotherapist how active you should aim to be.
Lung cancer doesn’t always cause symptoms in the early stages. But the first signs may be a cough that doesn’t go away or changes, coughing up blood, and shortness of breath. Other symptoms of lung cancer may include pain in your chest and feeling very tired. For more information, see our symptoms of lung cancer section.
Effects of smoking
Did our Lung cancer information help you?
We’d love to hear what you think. Our short survey takes just a few minutes to complete and helps us to keep improving our health information.
The health information on this page is intended for informational purposes only. We do not endorse any commercial products, or include Bupa's fees for treatments and/or services. For more information about prices visit: www.bupa.co.uk/health/payg
This information was published by Bupa's Health Content Team and is based on reputable sources of medical evidence. It has been reviewed by appropriate medical or clinical professionals and deemed accurate on the date of review. Photos are only for illustrative purposes and do not reflect every presentation of a condition.
Any information about a treatment or procedure is generic, and does not necessarily describe that treatment or procedure as delivered by Bupa or its associated providers.
The information contained on this page and in any third party websites referred to on this page is not intended nor implied to be a substitute for professional medical advice nor is it intended to be for medical diagnosis or treatment. Third party websites are not owned or controlled by Bupa and any individual may be able to access and post messages on them. Bupa is not responsible for the content or availability of these third party websites. We do not accept advertising on this page.
- Lung cancer statistics. Cancer Research UK. www.cancerresearchuk.org, accessed January 2025
- Lung and pleural cancer – recognition and referral. NICE Clinical Knowledge Summaries. cks.nice.org.uk, last revised February 2021
- Lung cancer: Diagnosis and management. NICE Guidance NG122. National Institute for Health and Care Excellence (NICE). www.nice.org.uk, last updated March 2024
- Lung anatomy. Medscape. emedicine.medscape.com, updated December 2017
- Types of lung cancer. Cancer Research UK. www.cancerresearchuk.org, last reviewed December 2022
- Small cell lung cancer. BMJ Best Practice. bestpractice.bmj.com, last reviewed November 2024
- Non-small cell lung cancer. BMJ Best Practice. bestpractice.bmj.com, last reviewed November 2024
- Non-small cell lung cancer (NSCLC). Medscape. emedicine.medscape.com, updated October 2024
- Lung carcinoma (lung cancer). The MSD Manuals. www.msdmanuals.com, reviewed/revised May 2023
- What is lung cancer? Cancer Research UK. www.cancerresearchuk.org, last reviewed December 2022
- What is secondary lung cancer? Cancer Research UK. www.cancerresearchuk.org, last reviewed August 2023
- Cough (acute): microbial prescribing. NICE Guidance NG120. National Institute for Health and Care Excellence (NICE). www.nice.org.uk, last updated February 2019
- Suspected cancer: recognition and referral. NICE Guidance NG12. National Institute for Health and Care Excellence (NICE). www.nice.org.uk, last updated October 2023
- Lung cancer in adults. NICE quality standard QS17. National Institute for Health and Care Excellence (NICE). www.nice.org.uk, last updated December 2019
- Computerised tomography (CT scans). Patient. patient.info, last updated October 2021
- PET-CT scan. Cancer Research UK. www.cancerresearchuk.org, last reviewed November 2022
- Bronchoscopy Cancer Research UK. www.cancerresearchuk.org, last reviewed July 2022
- Needle biopsy through the skin for lung cancer. Cancer Research UK. www.cancerresearchuk.org, last reviewed December 2022
- Stages and types of lung cancer. Cancer Research UK. www.cancerresearchuk.org, last reviewed December 2022
- Palliative care. Patient. patient.info, last updated September 2022
- Fitter Better Sooner. Royal College of Anaesthetists. www.rcoa.ac.uk, published November 2024
- General principles of radiation therapy. Medscape. emedicine.medscape.com, updated February 2022
- Chemotherapy for lung cancer. Cancer Research UK. www.cancerresearchuk.org, last reviewed December 2022
- Targeted and immunotherapy treatment for lung cancer. Cancer Research UK. www.cancerresearchuk.org, last reviewed March 2023
- Tepotinib for treating advanced non-small-cell lung cancer with met gene alterations. NICE Technology Appraisal Guidance TA789. National Institute for Health and Care Excellence (NICE). www.nice.org.uk, last updated May 2022
- Sotorasib for previously treated KRAS G12c mutation-positive advanced non-small-cell lung cancer. NICE Technology Appraisal Guidance TA781. National Institute for Health and Care Excellence (NICE). www.nice.org.uk, last updated March 2022
- Sotorasib [Specialist drug]. NICE British National Formulary. bnf.nice.org.uk, last updated November 2024
- Tepotinib [Specialist drug]. NICE British National Formulary. bnf.nice.org.uk, last updated November 2024
- Secondhand smoke. Action on Smoking and Health. ash.org.uk, published March 2020
- UK Chief Medical Officers Physical Activity Guidelines. Department of Health and Social Care. assets.publishing.service.gov.uk, published September 2019
- Coping and support when you have lung cancer. Cancer Research UK. www.cancerresearchuk.org, last reviewed March 2023
- Support at home for you and your family. Cancer Research UK. www.cancerresearchuk.org, last reviewed August 2023
- Choosing where to die. Macmillan Cancer Support. www.macmillan.org.uk, reviewed September 2022
- How to find a clinical trial. Cancer Research UK. www.cancerresearchuk.org, last reviewed February 2022
- After lung cancer surgery. Cancer Research UK. www.cancerresearchuk.org, last reviewed January 2023
- Hill W, Lim EL, Weeden CE, et al. Lung adenocarcinoma promotion by air pollutants. Nature 2023; 616(7955):159–67. doi: 10.1038/s41586-023-05874-3. Epub 2023 Apr 5. PMID: 37020004; PMCID: PMC7614604
- Klebe S, Rathi V, Russell PA. Lung cancer caused by asbestos: What a reporting pathologist needs to know. Lung Cancer 2024; 195:107849. doi: 10.1016/j.lungcan.2024.107849. Epub 2024 Jun 21. PMID: 39089005
- Personal communication, Dr James Wilson, Consultant Clinical Oncologist, January 2025
- Lung health checks. Cancer Research UK. www.cancerresearchuk.org, last reviewed January 2023
- Cancer. Earlier diagnosis. Targeted lung health checks. NHS England. www.england.nhs.uk, accessed January 2025
- Cancer clinical trials. Finding a cancer clinical trial. Macmillan Cancer Support. www.macmillan.org.uk, reviewed August 2022
- Palliative treatments. Cancer Research UK. www.cancerresearchuk.org, last reviewed November 2021
- Victoria Goldman, Freelance Health Editor


