Ovarian cancer
- Dr Joseph Yazbek, Consultant Gynaecologist and Gynaecological Oncology Surgeon
Ovarian cancer is when cells in or around your ovaries stop growing normally and start growing out of control. Any woman or person with ovaries can get this type of cancer.
About ovarian cancer
Ovaries are two small, oval organs in your pelvis. Your pelvis is the lower part of your tummy, between your hip bones. Your ovaries release an egg every month. This is usually in the middle of your period (menstrual cycle).
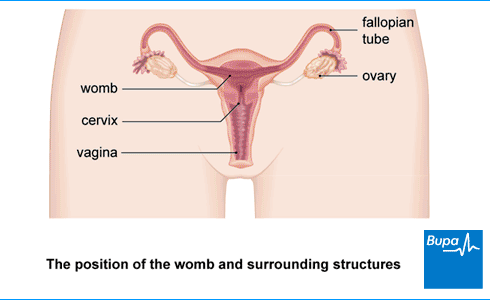
Ovarian cancer starts inside your ovary or fallopian tubes (the tubes that lead from your ovaries to your womb).
Sometimes, ovarian cancer can spread out of your ovary and fallopian tube. It may spread more widely in your tummy. More rarely, it can spread to other organs, such as your liver, lymph nodes, and lungs.
Ovarian cancer is the sixth most common cancer in women in the UK. Around 7,500 women are diagnosed with this type of cancer every year. It’s most common in those over 50, but you can get it when you’re younger too.
Types of ovarian cancer
There are several types of ovarian cancer. These start in different parts of your ovaries and are treated in different ways.
- Epithelial ovarian cancer is the most common type. It causes 9 out of 10 ovarian cancers. It starts in the cells that cover your ovaries and the ends of your fallopian tubes. There are different subtypes of epithelial ovarian cancer, named according to which type of cell is involved.
- Non-epithelial ovarian cancer is much less common. Again, there are different subtypes. The most common subtype grows from germ cells (the cells in your ovary that make eggs). This usually affects people under 35.
Borderline ovarian tumours tend to affect those aged 20 to 40. These are a type of epithelial tumour, and tend to grow more slowly than cancer cells. Borderline ovarian tumours are usually removed with surgery.
Your doctor will tell you which type of ovarian cancer you have, and how this will affect your treatment.
How cancer develops
Cancer explained | Watch in 1:48 minutes
In this video, we explain how, when cells divide uncontrollably, this leads to cancer.
Causes of ovarian cancer
Doctors don’t know the exact cause of ovarian cancer but certain things can make you more likely to get it. These include:
- a family history of ovarian or breast cancer, or some other cancers, especially if you inherit faulty genes called BRCA1 and BRCA2
- getting older – most people who get it are over 50
- hormone replacement therapy (HRT) – this seems to increase your risk by a small amount
- being overweight or obese
- endometriosis – if you have this condition, it increases your risk of some types of ovarian cancer by a small amount
- smoking
- if you started your periods early
- if you started the menopause late in life
Some things may make you less likely to get ovarian cancer. These include:
- taking the contraceptive pill
- having children – the more children you’ve had, the lower your risk
- breastfeeding your children
- having had a hysterectomy or been sterilised (had your tubes tied)
Symptoms of ovarian cancer
Many ovarian cancer symptoms are quite vague, and may be similar to symptoms caused by other, less serious conditions. And you might not get any early warning signs of ovarian cancer – you might not have any symptoms at all in the early stages of the disease. This means that by the time many people see their doctor, their cancer is already at quite an advanced stage.
If you do get ovarian cancer symptoms, the most common include:
- pain or discomfort in your tummy or pelvis
- a swollen tummy
- constantly feeling bloated
- feeling full quickly and losing your appetite
- needing to pee more often or more urgently
- unexplained changes in your poo (bowel habits), such as constipation, excess wind, or diarrhoea
- other symptoms that affect your digestive system, such as feeling sick or indigestion
Other ovarian cancer symptoms include:
- losing weight for no obvious reason
- unexplained extreme tiredness
- abnormal bleeding from your vagina (such as after you’ve gone through the menopause)
- feeling short of breath
If you do have any of the above symptoms, you have them regularly, and they last for longer than a few weeks, contact your GP.
Diagnosis of ovarian cancer
Your GP will ask you about your symptoms and medical history. They’ll examine you by feeling around your tummy and pelvis. They may ask to examine you internally too. In a vaginal examination, your doctor will put some gloves on and add some lubricant, then insert their fingers into your vagina. They’ll use their other hand to press lightly on your tummy (abdomen) and will gently feel for any abnormalities in and around your womb and ovaries.
Tests for ovarian cancer
Your GP may arrange for you to have a blood test to check for a protein called CA125. A high CA125 level can be a sign of ovarian cancer. But other conditions can raise your CA125 level too. If your level of CA125 is found to be higher than normal, your GP may arrange for you to have an ultrasound scan to check your tummy and pelvis.
Referral to a specialist
Depending on your test results, your GP may refer you to a gynaecologist (a doctor who specialises in women’s reproductive health). Sometimes, your GP may refer you to a gynaecologist urgently (within two weeks), before they do any more tests. They’ll then organise any tests and scans for you.
Staging tests
Your doctor will look at your blood test results and ultrasound to see how large your cancer is and how far it’s spread. Sometimes you’ll need other tests, such as a CT scan or MRI scan. Your doctor may recommend a procedure to remove a sample (biopsy) of your ovary to test for cancer cells.
Finding out how far your cancer has spread is called staging. Staging can help doctors to estimate how your cancer is likely to progress. It can also help them to decide on the best way to treat your cancer.
If your cancer is more advanced, your doctor will need to take tissue samples from the tumour. They may look at these with the CT scan to see the stage. Tissue samples are usually taken when the tumour is removed during surgery – see our treatment of ovarian cancer section.
Genetic testing
You should be offered genetic testing after you’re diagnosed with ovarian cancer – talk to your doctor about whether you’re eligible. This will check for faulty BRCA1 and BRCA2 genes. If you have these, it can increase your risk of both ovarian and breast cancer.
If you know whether you have the faulty BRCA genes, it may help your doctor to plan your treatment better. There are lots of things to think about before you have a genetic test – your doctor will talk you through what’s involved.
Looking for cancer cover that supports you every step of the way?
If you develop new conditions in the future, you can rest assured that our health insurance comes with full cancer cover as standard.
To get a quote or to make an enquiry, call us on 0800 600 500∧
Treatment of ovarian cancer
A multidisciplinary team (MDT) of specialist doctors, including a gynaecological oncologist (a surgeon who specialises in cancers that affect the female reproductive system), will be involved in planning your care. Other health professionals will include oncologists, radiologists, pathologists, and nurse specialists. They will advise you on your initial treatment and any other management going forward.
Which ovarian cancer treatment they recommend will depend on:
- the type of ovarian cancer you have
- whether it’s spread, and if so, how far
They’ll talk to you about all the possible options. And they’ll discuss anything that may affect your decision, such as:
- your general health
- whether you plan to have children
Surgery
Almost everyone with ovarian cancer has surgery to remove as much of the tumour as possible. This is called cytoreductive surgery, and usually involves removing:
- both of your ovaries
- your fallopian tubes
- your womb (a total hysterectomy)
Your gynaecological oncologist may also remove some surrounding tissue (take biopsies) and nearby lymph nodes. This will help them to find out how far the cancer has spread.
You may be able to just have the affected ovary and fallopian tube removed if your cancer hasn’t spread outside your ovary, and you want to have children in the future.
Chemotherapy
Most people with ovarian cancer have chemotherapy as well as surgery. Chemotherapy is a treatment for cancer that uses medicines to destroy cancer cells. It usually involves having several doses of chemotherapy medicines at regular intervals over a few weeks.
Most of the time, your doctor will offer you chemotherapy after surgery. This will destroy any cancer cells that weren’t removed by the operation. They may also offer you chemotherapy before surgery to shrink your tumour and make it easier to remove.
The exact chemotherapy treatment you’re offered will depend on the type and stage of your cancer. Your doctor will give you information about what’s best for you.
Radiotherapy
Radiotherapy uses radiation to destroy cancer cells. It’s not often used to treat ovarian cancer. But your doctor may offer it to shrink your cancer before surgery. Radiotherapy can also help to ease ovarian cancer symptoms, such as pain, if you can no longer have other treatments.
Targeted therapies
Other medicines for ovarian cancer include:
- monoclonal antibodies
- PARP (Poly ADP-ribose polymerase) inhibitors
These medicines target cancer cells to stop them growing and multiplying. These may have fewer side-effects than traditional chemotherapy. You may be offered this treatment if:
- you’ve been found to have a faulty BRCA gene
- your cancer is advanced
- your cancer has come back
After your treatment
You’ll have regular check-ups after your treatment has finished, to check how well your treatment has worked and see if the cancer has come back. It’s important to go to these appointments, even if you feel well. If your cancer has returned, your doctor will talk to you about any more treatment options you may try.
Prevention of ovarian cancer
You may be able to reduce your chances of getting ovarian cancer if you:
- stop smoking
- lose excess weight
- be more physically active
If you take these steps, it may help to reduce your risk of some other cancers too. They’re also important for your general health. But making changes to your lifestyle can’t completely prevent ovarian cancer. There are many things that you can’t control, such as your age and your genes.
If you have a strong family history, your GP may refer you to a genetic counselling clinic. This is usually if you have any close relatives who have had breast or ovarian cancer. Specialists at the clinic will assess your risk. They may test for the BRCA1 and BRCA2 faulty genes.
If you test positive for these genes, your doctor will talk to you about ways to reduce your risk of both breast and ovarian cancer. For ovarian cancer, you may be advised to:
- take oral contraceptives
- have regular ultrasound scans of your ovaries
- have surgery to remove your ovaries and fallopian tubes (risk-reducing surgery), depending on your age
Help and support
If you’re diagnosed with ovarian cancer, it’s important you have support, especially while you’re having treatment. This will help you deal with the:
- emotional side of having cancer
- practical issues
- physical symptoms
Specialist cancer doctors and nurses are experts in providing the support you need – make sure you talk to them if you’re worried about anything.
Talk to your family and friends as it can help them to understand what you’re going through and how you’re feeling. Organisations and support groups that specialise in ovarian cancer (see the other helpful websites section) can also be a great source of information and support.
You may also find it helpful to speak to someone else who has had ovarian cancer and been through treatment.
There aren’t always early warning signs of ovarian cancer. But early symptoms can include pain in your tummy or pelvis, a swollen or bloated tummy, feeling full quickly and needing to pee regularly.
See our symptoms of ovarian cancer section for more information.
The stage of a cancer means how big it is, and if it’s spread. How fast this happens can vary, depending on things like the type of cancer you have and the treatment you have, and when. It’s important to get a diagnosis as soon as possible to improve your chance of treating ovarian cancer successfully and stop it moving stages. If you have any ovarian cancer symptoms, see your GP.
See our symptoms of ovarian cancer section for more information.
How aggressive ovarian cancer is depends on the type of cancer. Cancer cells have mutations in their DNA (biological instructions you inherit, and which tell your cells what to do) that cause the cells to grow uncontrollably. Tumours that contain mutations in a gene called PTEN are thought to be more aggressive. These tumours seem to grow more quickly than those without PTEN mutations. Research is looking into this, which may eventually lead to more treatments.
Test for ovarian cancer include a blood test. This will check for the CA125 protein, which may be high in people with ovarian cancer. You may also have an ultrasound scan and other tests.
For more information, see our diagnosis of ovarian cancer section.
Chemotherapy
Hysterectomy
Gynaecological laparoscopy
In a gynaecological laparoscopy, your surgeon uses a camera (laparoscope) to see inside your lower abdomen (tummy). This means they will be able to see your womb (uterus), fallopian tubes and ovaries.
Did our Ovarian cancer information help you?
We’d love to hear what you think. Our short survey takes just a few minutes to complete and helps us to keep improving our health information.
The health information on this page is intended for informational purposes only. We do not endorse any commercial products, or include Bupa's fees for treatments and/or services. For more information about prices visit: www.bupa.co.uk/health/payg
This information was published by Bupa's Health Content Team and is based on reputable sources of medical evidence. It has been reviewed by appropriate medical or clinical professionals and deemed accurate on the date of review. Photos are only for illustrative purposes and do not reflect every presentation of a condition.
Any information about a treatment or procedure is generic, and does not necessarily describe that treatment or procedure as delivered by Bupa or its associated providers.
The information contained on this page and in any third party websites referred to on this page is not intended nor implied to be a substitute for professional medical advice nor is it intended to be for medical diagnosis or treatment. Third party websites are not owned or controlled by Bupa and any individual may be able to access and post messages on them. Bupa is not responsible for the content or availability of these third party websites. We do not accept advertising on this page.
- Ovarian cancer. BMJ Best Practice. bestpractice.bmj.com, last updated 12 March 2025
- Arora T, Mullangi S, Vadakekut ES, et al. Epithelial ovarian cancer. StatPearls Publishing. ncbi.nlm.nih.gov/books, last updated 6 May 2024
- Ovarian cancer. Patient. patient.info, last updated 4 June 2024
- Female reproductive organ anatomy. Medscape. emedicine.medscape.com, updated 27 November 2024
- Ovary anatomy. Medscape. emedicine.medscape.com, updated 28 January 2025
- Ovarian cancer. NICE Clinical Knowledge Summaries. cks.nice.org.uk, last revised August 2023
- Ovarian cancer statistics. Cancer Research UK. cancerresearchuk.org, accessed 9 April 2025
- Borderline ovarian tumours. Cancer Research UK. cancerresearchuk.org, last reviewed 27 November 2024
- Epithelial ovarian cancer. Cancer Research UK. cancerresearchuk.org, last reviewed 18 February 2025
- Ovarian cancer. Medscape. emedicine.medscape.com, updated 15 August 2024
- Symptoms of ovarian cancer. Cancer Research UK. cancerresearchuk.org, last reviewed 25 November 2024
- Diagnosing ovarian cancer. Cancer Research UK. cancerresearchuk.org, last reviewed 27 November 2024
- Genital examination in women. Royal College of Nursing. rcn.org.uk, last updated 6 November 2023
- Tests for ovarian cancer. Cancer Research UK. cancerresearchuk.org, last reviewed 28 November 2024
- Ovarian cancer: Identifying and managing familial and genetic risk. National Institute for Health and Care Excellence (NICE). nice.org.uk, published 21 March 2024
- Primary invasive breast cancer. BMJ Best Practice. bestpractice.bmj.com, last updated 28 November 2024
- Maximal cytoreductive surgery for advanced ovarian cancer. National Institute for Health and Care Excellence (NICE). nice.org.uk, published 5 April 2023
- Types of surgery for ovarian cancer. Cancer Research UK. cancerresearchuk.org, last reviewed 18 February 2025
- Chemotherapy for ovarian cancer. Cancer Research UK. cancerresearchuk.org, last reviewed 3 December 2024
- Radiotherapy for ovarian cancer. Cancer Research UK. cancerresearchuk.org, last reviewed 4 December 2024
- Causes of cancer and reducing your risk. Cancer Research UK. cancerresearchuk.org, accessed 15 April 2025
- Coping and support when you have ovarian cancer. Cancer Research UK. cancerresearchuk.org, last reviewed 5 December 2024
- About the stages and grades of ovarian cancer. Cancer Research UK. cancerresearchuk.org, last reviewed 28 November 2024
- Why are some ovarian cancer tumours particularly aggressive? Ovarian Cancer Action. ovarian.org.uk, accessed 14 April 2025
- Rachael Mayfield-Blake, Freelance Health Editor


