Colonoscopy
- Dr Derek Chan, Consultant Physician and Gastroenterologist
A colonoscopy is a test to investigate symptoms or check for conditions affecting your bowel, including bowel cancer. The large bowel is also known as the colon or large intestine.
The doctor uses a narrow, flexible, telescopic camera to look inside your large bowel (a colonoscope). The test can also look inside a part of the small bowel.
Why do I need a colonoscopy?
You may have a colonoscopy to investigate bowel symptoms, screen for polyps or cancers, or check for other conditions affecting the bowel. Or you may have one to monitor a bowel condition that has already been diagnosed.
Screening
You may have a colonoscopy as part of The National Bowel Cancer Screening Programme. In England and Scotland, bowel cancer screening is offered every two years to everyone aged from 53 to 74 years old. It is currently being extended to include people over 50. In Wales, screening is offered every two years to people aged 51 to 74 and in Northern Ireland, to people from 60 to 74.
The first stage of the screening programme is a kit you complete at home. This is called the faecal immunochemical test (FIT). You use this to collect a sample of poo. This is tested in a laboratory for traces of blood that you wouldn’t usually notice by looking at it. If blood is found in your poo, you’ll be offered a colonoscopy. This happens to about 2 in every 100 people who take the faecal immunochemical test.
Other reasons for a colonoscopy
Your doctor may recommend you have a colonoscopy for one of the following reasons.
You have symptoms that could indicate bowel cancer or another condition affecting the bowel. This includes:
- bleeding from your bottom
- a change in bowel habits (diarrhoea, constipation, or needing to poo more often)
You have a family history of bowel cancer. You are considered to be at increased risk of bowel cancer if you have a first-degree relative who has had it, particularly if they were diagnosed before they were 50. Having more than one first-degree relative with bowel cancer increases your risk further. A first-degree relative is a parent, brother, sister, or child.
You have inflammatory bowel disease (ulcerative colitis or Crohn’s disease) or have recently developed symptoms. You may also have colonoscopies to monitor or diagnose these conditions.
You’ve had a polyp or cancer removed. You may have a colonoscopy to make sure there are no more polyps. Or, to monitor your bowel if a rare condition called FAP runs in your family. This stands for familial adenomatous polyposis. It’s caused by a faulty gene and results in lots of pre-cancerous polyps developing in the bowel.
You need follow-up to another test, such as a CT scan or virtual colonography. This could be because you need further assessment or treatment.
If necessary, you can also have a tissue sample taken (a biopsy) or polyps removed during a colonoscopy. This is painless procedure.
Preparation for a colonoscopy
You’ll usually have a colonoscopy in the endoscopy unit at a hospital. Normally, you can go home the same day. Ask a friend or family member to drive you home, because you are likely to have some sedation. Sedation can make you feel drowsy for a while afterwards, so you won’t be able to drive until the day after.
Your hospital will tell you how to prepare for your colonoscopy. There is more information about this below.
When you arrive at the hospital, you will meet the endoscopist. This is the person who will carry out your colonoscopy and may be a doctor or specially trained nurse. They will explain what will happen and what to expect afterwards. They’ll also tell you about possible complications.
Your endoscopist will assess whether you are fit enough to have a colonoscopy. Tell them if you’re pregnant, breastfeeding, or have any health conditions.
If your colonoscopy is part of the screening programme, you’ll have an appointment with a specialist screening practitioner. They will talk through the procedure and possible results.
Be sure to ask any questions you have and ask for more time to make a decision if you need to. If you’re happy to go ahead with the procedure, you need to sign a consent form.
Medicines
There are some medicines that you need to stop taking before you have a colonoscopy. These include:
- iron tablets – stop taking these one week before your colonoscopy
- anti-diarrhoea medicines or any medicines that may cause constipation – stop taking these one to two days before your colonoscopy
- medicines that affect the way your blood clots (for example, warfarin or clopidogrel) – you usually stop taking these five days before your colonoscopy, but this depends on which medicine you are taking and why you are taking them. Always follow the advice of your doctor
If you are taking any other medicines, ask your GP whether you need to stop taking them before the colonoscopy.
Clearing your bowel
Your bowel needs to be completely empty so that your endoscopist can see everything clearly. Your hospital will give you a strong laxative to take. You normally take this both the day before and on the morning of your test. It usually comes as a powder that you mix with water. Let your hospital know if you’re pregnant or breastfeeding as you may not be able to take the laxative.
You will have full instructions of what to do, but you usually drink the solution over an hour. It starts to work very quickly. So make sure you stay close to a toilet after you take it. You might feel some discomfort or bloating in your tummy (abdomen).
Taking the laxative is not pleasant. But it’s really important to clear your bowel before the procedure. It may help to put the mixture in the fridge beforehand.
Your hospital will give you advice about what you can eat or drink before the procedure. They may ask you to eat only low-fibre foods, or not to eat at all, for at least a day beforehand. It’s important to keep drinking plenty of clear fluids like water, squash or black tea, or coffee. This will make sure you don’t get dehydrated.
If you take the contraceptive pill, laxatives will prevent it being absorbed. Follow the instructions in the patient information leaflet for your contraceptive pills. You may need to use another form of contraception, such as a condom, for a while.
The preparation for a colonoscopy can vary, particularly if you have any health conditions such as diabetes. So, follow the instructions your hospital gives you, and ask if you’re not sure about anything.
At the hospital
When you arrive at the hospital, you’ll see a nurse or doctor and can ask them any final questions. They’ll give you a hospital gown to wear and sometimes a pair of paper shorts that open at the back.
Colonoscopy procedure
A colonoscopy usually takes around 30 to 45 minutes, although the appointment itself will probably last around two hours.
You don’t have an anaesthetic for a colonoscopy, but may have a painkiller and sedation. This is because the procedure can be uncomfortable.
A sedative will make you feel more relaxed and a bit drowsy, but you’ll be awake throughout the procedure. You have the sedative as an injection into a vein in your arm or hand at the start of the procedure. Your doctor may offer you gas and air (Entonox) instead of a sedative. However, you may not be able to have Entonox if you have asthma or another breathing condition.Your endoscopist (doctor or nurse) will ask you to lie on your left-hand side and bend your knees. First, they’ll gently examine your bottom with their finger. They’ll then carefully put in the colonoscope. They’ll use a lubricating gel to make this as comfortable as possible. The tube (for adults) is only around 1cm in diameter so will usually go in easily.
Your endoscopist will put some air or water into your bowel through the colonoscope. This inflates your bowel slightly to give them a better view of the bowel lining. This can make you feel a little bloated. They’ll then gently guide the colonoscope through your bowel. The images from the camera at the end of the colonoscope will appear on a monitor screen.
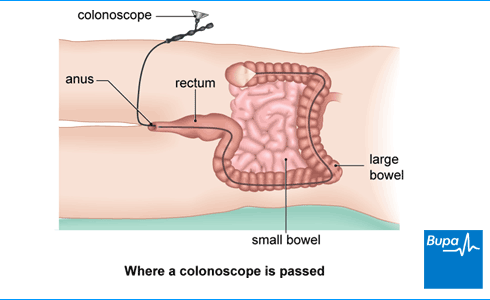
Your endoscopist might ask you to change position during the procedure. This helps them to reach and examine different areas of your bowel. They may also press on your tummy to help move the colonoscope in the right direction.
Your endoscopist may take a small sample of cells (a biopsy) if needed. They may remove any growths (polyps) they find. They’ll pass instruments through the colonoscope to do this.
If you find the procedure particularly uncomfortable at any stage, tell your endoscopist. They’ll stop or change what they’re doing.
Aftercare for colonoscopy
If you’ve had sedation for your colonoscopy, a nurse will monitor you for an hour or so afterwards. They need to make sure the immediate effects of the sedative have worn off. After that, you should be fine to go home when you feel ready. Ask someone to take you home and stay with you overnight while the sedative wears off completely.
Before you leave, your doctor or nurse may talk to you about the colonoscopy. They’ll tell you whether they’ve removed any polyps or taken any biopsies. They may also give you a copy of the colonoscopy report. If you’ve had a biopsy or polyps removed, they’ll tell you how and when you can expect to receive your results. It’s usually within two weeks.
Access Bupa services without health insurance
With our pay as you go healthcare you can pay for the treatment you need, when you need it. It’s fast, flexible and you don’t need health insurance.
Recovery for colonoscopy
You may feel bloated and have some cramping pain after a colonoscopy. This is caused by the gas used during the procedure and usually settles down within a few hours.
If you need to, you can take over-the-counter medicines, such as paracetamol or ibuprofen. If you’ve had a biopsy or a polyp removed, you may also bleed a little from your bottom. This should stop within a couple of days – contact your GP or the hospital if it doesn’t.
Having sedation can make you tired. You might find that you’re not as co-ordinated as usual or that it's difficult to think clearly. This should pass within 24 hours. During this time don't:
- drive
- drink alcohol
- operate machinery
- make any important decisions or post on social media
Complications of colonoscopy
Colonoscopy is carried out very often and is a safe procedure. However, with any medical procedure it is possible to complications to occur. The main possible complications of a colonoscopy are listed below.
- You may have a reaction to the sedation that affects your breathing. You will be monitored throughout, and can have treatment if this does happen.
- A tear in your bowel (perforation), caused by the colonoscope is rare. It happens to fewer than 1 in 1,500 people. If it does happen, you may need surgery to repair it.
- Bleeding is most likely to happen after having biopsies or polyps removed and usually stops on its own. In fewer than 1 in 2,000 people it can become serious and need a blood transfusion.
Contact the hospital department where you had your procedure if:
- you continue to bleed from your bottom
- have severe pain in your tummy that doesn’t get better within a couple of days
Alternatives to colonoscopy
A colonoscopy is usually the best investigation to see inside your bowel because it can examine the whole of your large bowel. Your doctor can also take biopsies and remove polyps if necessary. But it isn’t suitable for everyone so your doctor might suggest other tests. Other options include the following.
- Virtual colonoscopy involves having a CT scan of your large bowel after gas is passed into your bowel to expand it.
- Flexible sigmoidoscopy is similar to a colonoscopy but uses a shorter instrument to look inside only the lower part of your large bowel.
- Barium enema involves taking X-ray images of your large bowel. A contrast or dye (barium) is put into your bowel to show up the detail and give clearer X-ray images.
- In colon capsule endoscopy, you swallow a capsule containing a tiny video camera. This takes digital pictures and transmits them wirelessly as it passes through your bowel. This new treatment isn’t yet available in all hospitals.
If you have one of these tests, you may still need a colonoscopy to take a closer look at your bowel.
You may feel bloated and have some cramping pain for a few hours after a colonoscopy. This is because of the gas used during the procedure. You can take over-the-counter medicines, such as paracetamol or ibuprofen. If you have a sedative, you might feel tired but you should recover within 24 hours.
For more information, see our section on recovery from colonoscopy.
A colonoscopy can check your large bowel for any signs of bowel cancer. It’s used in bowel cancer screening programmes. It can also investigate any bowel-related symptoms. This helps your doctor diagnose conditions, such as ulcerative colitis or Crohn’s disease. It can also be used to monitor your bowel if you’ve been diagnosed with these already.
For more information, see our section on why do I need a colonoscopy?
Yes, you’ll be awake for a colonoscopy, but you may be sedated. This will make you feel more relaxed and drowsy and you may doze off. Some hospitals offer gas and air (Entonox) instead of a sedative.
For more information, see our section on colonoscopy procedure.
The laxative will give you diarrhoea, so make sure you stay close to a toilet after you take it. How long you’ll have diarrhoea can vary. Plan to stay at home for a few hours at least.
For more information, see our section on preparation for a colonoscopy.
A standard colonoscope (for use in adults) is a long flexible tube that’s about 1cm wide. You won’t need an anaesthetic for a colonoscopy. But the procedure can be uncomfortable, so you may have painkillers and sedation.
For more information, see our section on colonoscopy procedure.
Polyps are small lumps that can develop in the lining of your bowel. They don’t usually cause any problems but sometimes, over time, a type of polyp will grow into a cancer. If your doctor finds any polyps during your colonoscopy, they’ll remove them. If you have polyps, you may need regular colonoscopies in future to check for any more.
For more information, see the section on why do I need a colonoscopy?
Bowel cancer
Bowel cancer (or colorectal cancer) is the name for any cancer that starts in your large bowel, rectum (back passage) or appendix.
Crohn's Disease
Crohn’s disease is an inflammatory condition that affects your gastrointestinal tract.
Ulcerative colitis
Ulcerative colitis is a condition that affects your large bowel and rectum (back passage).
Did our Colonoscopy information help you?
We’d love to hear what you think. Our short survey takes just a few minutes to complete and helps us to keep improving our health information.
The health information on this page is intended for informational purposes only. We do not endorse any commercial products, or include Bupa's fees for treatments and/or services. For more information about prices visit: www.bupa.co.uk/health/payg
This information was published by Bupa's Health Content Team and is based on reputable sources of medical evidence. It has been reviewed by appropriate medical or clinical professionals and deemed accurate on the date of review. Photos are only for illustrative purposes and do not reflect every presentation of a condition.
Any information about a treatment or procedure is generic, and does not necessarily describe that treatment or procedure as delivered by Bupa or its associated providers.
The information contained on this page and in any third party websites referred to on this page is not intended nor implied to be a substitute for professional medical advice nor is it intended to be for medical diagnosis or treatment. Third party websites are not owned or controlled by Bupa and any individual may be able to access and post messages on them. Bupa is not responsible for the content or availability of these third party websites. We do not accept advertising on this page.
- Colorectal surgery. 2nd ed. Oxford Medicine Online. academic.oup.com, published online August 2021
- The bowel. Bowel Cancer UK. bowelcanceruk.org.uk, last reviewed August 2024
- Bowel cancer screening: Having a colonoscopy. NHS England. gov.uk, last updated July 2022
- Bowel cancer screening: Programme overview. NHS England. gov.uk, last updated July 2024
- Bowel screening. Nice Clinical Knowledge Summaries. cks.nice.org.uk, last revised April 2024
- D'Souza N, Brzezicki A, Abulafi M. Faecal immunochemical testing in general practice. Brit J Gen Pract 2019; 69(679):60–61, published February 2019
- Bowel cancer screening: Helping you decide. NHS England. gov.uk, last updated July 2024
- Colorectal cancer. BMJ Best Practice. bestpractice.bmj.com, last updated: July 2024
- Family history. Bowel Cancer UK. bowelcanceruk.org.uk, last updated December 2019
- Hospital tests. Bowel Cancer UK. bowelcanceruk.org.uk, last reviewed May 2024
- Colonoscopy. Cancer Research UK. cancerresearchuk.org, last reviewed August 2022
- Clinical Endoscopist Training Programme. Health Education England. hee.nhs.uk, accessed September 2024
- Professional Standards: Decision making and consent. General Medical Council. gmc-uk.org, published November 2020
- Macrogol 3350 with anhydrous sodium sulfate, potassium chloride, sodium bicarbonate and sodium chloride. Nice British National Formulary. bnf.nice.org.uk, accessed September 2024
- Colonoscopy periprocedural care. Medscape. emedicine.medscape.com, last updated July 2024
- Microgynon 30 tablets. Electronic Medicines Compendium. medicines.org.uk, last updated February 2023
- Anaesthesia Explained. Royal College of Anaesthetists. rcoa.ac.uk, published March 2021
- Entonox (gas and air) in the endoscopy unit. Guy's and St Thomas' NHS Foundation Trust. guysandstthomas.nhs.uk, published June 2022
- Colonoscopy – A Guide to the Test. Northern Lincolnshire and Goole NHS Foundation Trust. nlg.nhs.uk, last updated April 2022
- Stauffer CM, Pfeifer C. Colonoscopy. StatPearls Publishing. ncbi.nlm.nih.gov, last updated July 2023
- Sedation explained. Royal College of Anaesthetists. rcoa.ac.uk, published June 2021
- Colorectal cancer. BMJ Best Practice. bestpractice.bmj.com, last updated: July 2024
- Colonoscopy Technique. Medscape. emedicine.medscape.com, last updated July 2024
- Flexible sigmoidoscopy. Medscape. emedicine.medscape.com, last updated February 2024
- Barium x-ray. Cancer Research UK. cancerresearchuk.org, last reviewed July 2022
- Capsule endoscopy technique. Medscape. emedicine.medscape.com, last updated November 2023
- Bowel cancer screening. Bowel Cancer UK. bowelcanceruk.org.uk, last reviewed May 2024
- Colon polyps – Beyond the Basics. UpToDate. uptodate.com, last updated January 2024
- Liz Woolf, Freelance Health Editor


