Gastric bypass surgery
- Mr Peter Lamb, Consultant General and Upper Gastrointestinal Surgeon
Gastric bypass surgery is an operation to help you lose weight if you’re very overweight. The surgery makes your stomach smaller and bypasses part of your bowels (intestines). Losing weight can help to improve any weight-related health problems you have.
About gastric bypass surgery
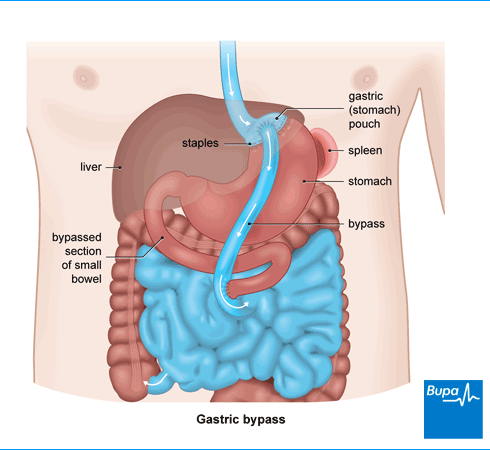
In gastric bypass surgery, your surgeon will section off part of your stomach and connect it directly to your small bowel. Food you eat will then bypass most of your stomach and the first part of your small bowel. You’ll feel fuller after eating smaller amounts of food. Gastric bypass surgery also changes hormone signals, including GLP-1, that pass between your bowel and your brain, which control your appetite.
You may hear this operation called a ‘Roux-en-Y’. This is the name of the method surgeons most often use to do it.
Gastric bypass surgery can help you lose up to two-thirds of your excess weight. You’re likely to lose most weight in the first year after surgery. You should be able to keep most of this weight off long-term. But this will depend on sticking to some major changes to your lifestyle after the operation. For example, you’ll need to:
- change your diet – stop snacking and choose healthier options
- not drink too much alcohol
- take regular exercise
Your doctor will talk through these changes with you.
Uses of gastric bypass surgery
Your GP may refer you to a specialist team to discuss your options. This is called a weight management service and includes a surgeon, dietitian, and psychologist. They’ll assess you to see if gastric bypass surgery is right for you. They may suggest weight loss surgery if you:
- have a body mass index (BMI) of 40 or more
- have a BMI over 35, with or without a condition that could improve if you lose weight (for example, type 2 diabetes or high blood pressure)
- are fit enough to have an anaesthetic and surgery
- are committed to having long-term follow-up appointments
- commit to changing your lifestyle and diet after your operation
- are over 18 (although children may have this surgery in exceptional circumstances)
You can usually only have gastric bypass surgery if you’ve tried to lose weight in other ways and this hasn’t worked. If you don’t meet the criteria for NHS funding, you may be able to have gastric bypass surgery privately.
Preparation for gastric bypass surgery
Your hospital will let you know how to prepare for your operation.
If you smoke, you’ll be asked to stop at least six weeks before the operation. Smoking increases your risk of complications after surgery.
Your surgeon may ask you to eat a low-fat, low-carbohydrate diet for two weeks before gastric bypass surgery . This will help to shrink your liver, which will allow your surgeon better access to your stomach.
You have gastric bypass surgery under a general anaesthesia (GA), so you’ll be asleep during the operation. You won’t be able to eat or drink for some time before surgery. Your doctors will tell you what to do – it’s important to follow their advice.
Your surgeon will ask you to wear compression stockings after the operation. This will help to prevent blood clots forming in the veins in your legs (deep vein thrombosis). You may also have injections of an anti-clotting medicine.
Your surgeon will discuss with you what will happen before, during, and after gastric bypass surgery . If you’re unsure about anything, ask. It’s important that you feel fully informed, so you feel happy to give your consent for the operation to go ahead. You do this by signing a consent form.
Gastric bypass surgery
A gastric bypass operation usually takes around two hours. But this can vary between hospitals.
Most surgeons use keyhole (laparoscopic) surgery. This means your surgeon will make several small cuts in your tummy rather than one large cut. They’ll put small instruments through the cuts and guide them using a telescope with a camera. Your surgeon may start with keyhole surgery and switch to open surgery if needed, but this isn’t common.
During the operation, your surgeon will staple across the top of your stomach, to form a small pouch. They’ll make an opening in the pouch and connect it directly to your small bowel. Food passing through will then bypass the lower part of your stomach and the first part of your small bowel. Your surgeon will reconnect the first part of your small bowel further down. This means the juices from your stomach, pancreas, and liver can mix with the food so that you can absorb nutrients after gastric bypass surgery .
Your surgeon will close your cuts with stitches and cover them with a dressing.
Aftercare for gastric bypass surgery
After gastric bypass surgery , you’ll need to rest until the anaesthetic has worn off. But it’s important to get out of bed and move around as soon as you can. This will help you to recover and prevent blood clots developing in your legs. Your doctor will prescribe you some painkillers.
Your hospital will take measures to help prevent deep vein thrombosis (DVT). You may have to wear compression stockings. Or you may have an intermittent compression machine that inflates and deflates around your legs. Both of these aim to boost the blood circulation in your legs. You may also continue to have anti-clotting injections, such as heparin.
As soon as you’re awake, you can start to drink small amounts of water.
Going home
You’ll usually be able to go home a day or two after your operation. Ask a friend or family member to drive you. Before you go home, your nurse will tell you how to care for your wounds and give you a follow-up appointment. You may need to take painkillers for a few days after the operation.
You usually go home on a liquid diet – your surgeon will give you advice on how to move on from this. There’s more information on diet below, in our section on recovery.
Recovery following gastric bypass surgery
Everyone recovers at their own rate, but allow up to six weeks to recover fully from a gastric bypass operation.
You have to make major changes to your lifestyle and diet after gastric bypass surgery, as your stomach will be smaller. You have a liquid diet for the first couple of weeks after you get home. Then you move on to puréed, then mashed food. By six weeks after your operation, you should be able to have several small solid meals a day.
It can be difficult to drink enough. You need at least one and a half to two litres a day to stay healthy. Drink slowly and between meals or it will fill you up too much.
Make sure you get enough protein every day. If you don’t, it can affect your health. Your doctor is likely to suggest a low-fat, high protein diet.
It’s difficult to get enough vitamins and minerals from your diet after gastric bypass. So you’ll need to take a complete multivitamin supplement for the rest of your life. You may also have regular vitamin B12 injections. Your doctor will arrange regular blood tests to check you’re getting everything you need.
You’ll need to do more exercise and drink less alcohol too. This will help you to get the most from your gastric bypass operation, so you can lose excess weight and keep it off.
Losing weight after a gastric bypass is usually a positive thing. But you may find it hard to adapt to your lifestyle and appearance after the operation. Talk to your GP or surgeon if you’re struggling to cope. They may suggest a patient support group. There you can get advice from other people who have been through the same operation.
Side-effects of gastric bypass surgery
You may have some bruising around your wounds after a gastric bypass. But this shouldn’t last more than a week or two.
You may feel sick or even be sick after eating. This is because you’ll only be able to eat a small amount of food at a time. This should get better with time as you get used to eating smaller amounts.
You may get an unpleasant side-effect called dumping syndrome if you eat too many sugary foods. It can make you feel sweaty, sick and lightheaded. You may also feel very tired and have tummy pain and diarrhoea. Symptoms can come on 30 minutes to an hour after you eat (early dumping), or within three hours (late dumping). It may help to:
- eat smaller more frequent meals that are low in carbohydrates, especially sugar
- don’t drink during meals or for half an hour afterwards
- cut down or cut out dairy products
- rest for half an hour after eating
Ask your dietitian or doctor for more advice.
Complications of gastric bypass surgery
Gastric bypass complications can happen soon after surgery or some months later. Early complications happen within a month of surgery. They include bleeding or a leak from the stomach or bowel. This is most likely where the stomach has been stapled or your small bowel rejoined. If you have tummy or shoulder pain, see signs of blood when you’re sick, or your poo looks black like tar, contact your surgeon or hospital.
Later complications can include the following.
- Gallstones – this can happen to one in three people who have this type of operation.
- • An internal hernia – part of the small bowel can get twisted at the site of the operation, which causes pain and you might require emergency surgery.
- Stomach ulcer – you may have a medicine to reduce stomach acid to help prevent this. Ulcers are more common in smokers.
- • A stricture – this is narrowing of the join between your stomach pouch and small bowel. You may feel sick, or be sick.
If you have pain, sickness that doesn’t go away, or any other concerns after your gastric bypass surgery , contact your surgeon for advice.
These complications may sound frightening, but, apart from gallstones, they are uncommon, particularly after keyhole surgery. Ask your surgeon to talk them through with you. They’ll give you more information about how likely they are for you.
Considerations for gastric bypass surgery
Gastric bypass surgery is a major operation with potentially serious complications. But it does also have many benefits. It’s important to discuss the surgery thoroughly with your doctor or surgeon beforehand. Then you can make an informed decision about whether to go ahead.
Benefits
Your doctor may suggest gastric bypass surgery to improve your overall health. Afterwards, you’re less likely to have:
- diabetes – surgery can reverse type 2 diabetes in many people
- breathing disorders, such as sleep apnoea
- a heart attack or stroke
- back pain and joint problems such as osteoarthritis
- high blood pressure
- weight-related cancers, such as womb cancer
For some people, gastric bypass surgery can help their mental health, with improved quality of life and less depression.
Drawbacks
You might not lose enough weight after gastric bypass surgery, or put weight back on later. Some people find it difficult to adapt to diet advice and lifestyle changes. Your surgeon will discuss this with you and support you.
You’ll need at least two years of medical care and check-ups after gastric bypass surgery . The changes to your lifestyle, along with what and how much you eat, are life-long commitments. You will also need to take vitamin and mineral supplements for the rest of your life.
Some people are disappointed with how they look after their operation. This is often because they’re left with excess skin. You may need further surgery to remove this but it may not be possible to have this on the NHS. It’s important to have realistic expectations, so talk to your surgeon beforehand.
Alternatives to gastric bypass surgery
There are medicines that can help with weight loss – ask your doctor for information about these.
Other types of surgery can help you lose excess weight. These include gastric sleeve surgery (gastrectomy) and gastric band surgery. As with gastric bypass surgery, you need to make long-term changes to your diet and lifestyle.
Another option is to have a silicone balloon inflated in your stomach. This will make you feel full but it can only be used short term.
Ask your doctor about the options available – they’ll help you decide which one is best for you.
It usually takes up to six weeks to recover from a gastric bypass surgery but everyone recovers at their own rate.
For more information, see the recovery following gastric bypass surgery section.
You’ll have to make major changes to your lifestyle and diet after gastric bypass surgery. You won’t be able to eat big meals after the operation, and you’ll need to avoid eating large amounts of sugary foods. This can cause dumping syndrome and make you feel ill. If you make the necessary lifestyle changes, it will help you to get the most from your gastric bypass operation, so you can lose excess weight and keep it off.
For more information, see the recovery following gastric bypass surgery section.
In gastric bypass surgery, your surgeon will section off part of your stomach and connect it directly to your small bowel. Food you eat will then bypass most of your stomach and the first part of your small bowel. You’ll feel fuller after eating smaller amounts of food. Gastric bypass surgery also changes hormone signals that pass between your bowel and your brain, which control your appetite.
For more information, see the about gastric bypass surgery section.
As with any operation, there are risks of gastric bypass surgery. But for most people, the risk of being obese and its related complications to health outweigh the risks of surgery. Gastric bypass surgery can improve your overall health. Afterwards, you’re less likely to have conditions such as diabetes and high blood pressure, which will help you to live a longer life.
For more information, see the considerations for gastric bypass surgery section.
Gastric band operation
Gastric band surgery is a common type of weight loss (bariatric) surgery for people who are very overweight (obese).
Tips for a healthy and well-balanced diet
A healthy, well-balanced diet involves eating foods from a variety of food groups to get the nutrients that your body needs to function.
Tools and calculators
BMI calculator
BMI, or body mass index, is one way of measuring whether you’re a healthy weight for your height.
Simply enter your details into our calculator and the result will give you an indication of whether you're a healthy weight.
Calories calculator
If you want to lose weight, you need to increase your physical activity and watch your calorie intake. Bupa's calorie calculator will help you to work out how many calories you're burning in a day.
Other helpful websites
Sources
- Overweight and obesity management. National Institute for Health and Care Excellence (NICE). nice.org.uk, published 14 January 2025
- Bariatric surgery. Patient. patient.info, last edited 25 April 2023
- Roux-en-y gastric bypass. StatPearls Publishing. Mitchell BG, Collier SA, and Gupta N. ncbi.nlm.nih.gov/books, last updated 9 November 2024
- Bariatric surgery sequelae. BMJ Best Practice. bestpractice.bmj.com, last reviewed 27 September 2025
- Bariatric surgery. Medscape. emedicine.medscape.com, updated 16 March 2023
- Metabolic and bariatric surgery. MSD Manual Professional Version. msdmanuals.com, reviewed/revised October 2025
- Grover R, Fortune BE, and Tow CY. The impact of alcohol on patients after bariatric surgery. Clin Liver Dis 2024; 23(1):e0139. doi: 10.1097/CLD.0000000000000139
- Roux-en-y gastric bypass (RYGB) surgery. Royal Berkshire NHS Foundation Trust. royalberkshire.nhs.uk, published April 2024
- Counseling patients on bariatric surgery for obesity. StatPearls Publishing. Wilson C. statpearls.com, last updated 18 September 2022
- Stenberg E, Dos Reis Falcão LF, O’Kane M, et al. Guidelines for Perioperative Care in Bariatric Surgery: Enhanced Recovery after Surgery (ERAS) Society recommendations: A 2021 update. World J Surg 2022; 46(4):729–51. doi: 10.1007/s00268-021-06394-9
- O'Kane M, Parretti H, Pinkney J, et al. British Obesity and Metabolic Surgery Society guidelines on perioperative and postoperative biochemical monitoring and micronutrient replacement for patients undergoing bariatric surgery – 2020 update. Bariatric surgery 2020; 21(11) doi: org/10.1111/obr.13087
- Laparoscopic gastric bypass. Medscape. emedicine.medscape.com, updated 26 April 2023
- Venous thromboembolism in over 16s: Reducing the risk of hospital-acquired deep vein thrombosis or pulmonary embolism. National Institute for Health and Care Excellence (NICE). nice.org.uk, last updated 13 August 2019
- Edwards MA, Powers K, Vosburg RW, et al. American Society for Metabolic and Bariatric Surgery: Postoperative care pathway guidelines for Roux-en-y gastric bypass. Surg Obes Relat Dis 2025 21(5):523–36. doi: 10.1016/j.soard.2025.01.005
- Bariatric surgery malnutrition complications. StatPearls Publishing. Ganipisetti VM. statpearls.com, last updated 19 May 2023
- Dumping syndrome. StatPearls Publishing. Hui C and Bauza GJ. statpearls.com, last updated 26 June 2023
- Dumping syndrome. Guts UK. gutscharity.org.uk, published August 2025
- Rachael Mayfield-Blake, Freelance Health Editor


